Akanksha, a housemaid, listens to her favorite songs on her husband’s phone after a long day at work. In a Mumbai slum, a very pregnant Dolly watches a YouTube video telling her how to prepare for delivering her baby. Satish, a street-food seller in Delhi, checks his day’s earning on PayTM, a digital payment app he recently installed on his data-enabled phone.
These are just a few examples of how the digital revolution is percolating into underserved, low-income communities in urban India. Digitally aligned government policies and a vibrant private sector are driving a rapidly evolving and economically inclusive digital ecosystem that even low-income users can afford. This newfound access has the potential to help address the health care needs of millions of underserved consumers. This is important because Indians pay 70 percent of health care expenses out of pocket. And in light of an overwhelmed health care infrastructure and rising rates in infectious and lifestyle disease, low-income populations in particular tend to lack access to adequate and appropriate health care.

One prudent way to address this challenge is to channel the reach of digital interfaces to equip low-income communities with the knowledge and resources to drive preventative health. However, embedding health care into digital tools requires that providers overcome contextual barriers and undertake deliberate design processes. To succeed, providers must develop a nuanced understanding of the obstacles to consuming information digitally, as well as glean insights from technology, interface design, and behavioral science.
Last year, our team conducted research on the digital usage patterns of underserved groups in two urban areas of India, and iteratively tested user interface and content design. Our work made young, low-income urban parents a strategic focal point, because they are recent adopters of the digital wave and have significant maternal and child health care needs. We generated primary research insights from more than 250 new mothers and fathers living in low-income communities, informing our understanding of the core barriers and digital needs of this population. Next, a multidisciplinary design team of IT experts, behavioral scientists, health care professionals, designers, and user researchers co-designed a mobile prototype for maternal and child health information. Iterative field testing, interviews, and analytics guided the adaptation of the prototype. The next generation of this application will launch later this year, reaching 5,000 families in a low-income community in Mumbai.
Here are some of the insights and learning garnered from our work:
- Cost is no longer the biggest barrier. The cost of phone ownership and data have long been beyond the economic means of the urban poor. However, in the last year, a strong government regulatory authority has promoted competition and consumer benefits that have rapidly driven down both smartphone and data costs, and ownership of data-enabled phones is now close to saturation among urban individuals with a monthly household income of more than $300.
- Infrastructure can overcome any remaining cost barriers: Remarkably, our data shows that only 5 percent of people living in less-connected and -developed localities owned smartphones, compared to a significant 56 percent of individuals with similar incomes living in neighborhoods with good mobile network and infrastructure (such as access to electricity). This finding confirms cost is not the primary determining factor in smartphone ownership. It also exemplifies the importance of digital exposure, accessibility, and infrastructure in connecting a population eager to access digital services.
- Digital experiences are not often built for low-income, urban populations. The most pervasive barrier to digital adoption in India today is a lack of knowledge about how to use digital interfaces. Even the switch from a basic phone’s T9 keyboard to an on-screen QWERTY keyboard can be a big challenge for users. Language also presents a barrier. India has an overall literacy rate of 74 percent. However, only about 10 percent of Indians can communicate in English—the language of the Internet. Local language content is scarce. And even when it’s available, it’s translated from original content written for an English-speaking audience, and doesn’t take into account local sensibilities and relevance. Further, interaction with a primarily text-based digital interface is a challenge for a population that, while literate by definition, is not as comfortable with the written form. For example, the spelling variations typed in by users for a search word like caesarean run into hundreds. These include cesarean, sigerian, cejaring, caeser, shejar, sijar, sejar, scissor, scissoring, and sizer—all terms that won’t retrieve the information someone looking for information on caesarean delivery needs. There are gaping holes in the understanding of early-stage user requirements and pain points, from both the digital interface and content experience perspectives.
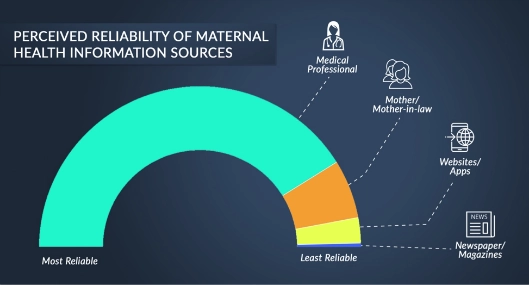
- There is a lack of trust in health-related digital information. For information on pregnancy and child health, for example, families traditionally seek out and trust doctors’ advice, as well as advice from their mothers. Low-income, underserved communities who have not been exposed to authentic digital content often have extreme distrust in digital information pertaining to health. Much of this distrust traces back to the absence of health information and services standards, both online and offline. In our research, only 12 percent of families thought information from digital sources was reliable, compared to more than 90 percent finding information from doctors and mothers to be most, very, or somewhat reliable.
Developing desire, trust, and mental capacities to use digital interfaces for inclusive health care is a multifaceted challenge. To truly meet the needs of underserved consumers, providers must focus on the following areas: high-quality content, behavior change, technology, and the structure of their design teams.
 Low-income communities who have not been exposed to authentic digital content often have distrust in digital information pertaining to health.
Low-income communities who have not been exposed to authentic digital content often have distrust in digital information pertaining to health.
High-quality content: To engage users on digital platforms, providers must use differentiated content that connects with a user’s specific journey. The form, tone, and continuity of content matters. Our testing of health content showed that video formats optimized for small, low-quality displays are most effective in driving engagement, primarily because they bypass literacy barriers, incorporate multiple auditory and visual sensory stimuli, and allow for easier comprehension and retention of information. When visual formats are not feasible, audio formats are the next best alternative. The voice delivering the content is most effective when it’s friendly and reassuring, and delivered in a local communication style. It’s also important to understand the environments in which users consume health content. For example, the volume of audio that seems appropriate in local labs can be too quiet to hear in places with high ambient noise. Finally, including local elements in the content, such as referring to local health clinics or the local grocery (kirana) stores, creates a link with users that helps win their trust.
Behavior change: Engaging users is vital to directing changes in consumer health behavior. For example, getting users to consume more nutritious food or recognize warning signs to go to the clinics requires that providers build a linear, intuitive, and cognitively light user experience. It’s important to be deliberate about the design of the user journey. This includes keeping screens uncluttered and sometimes using visuals with audio voiceovers to nudge the user forward. Providers must avoid paralyzing users with choices they may or may not be ready to make.
 Design interfaces need to be minimalistic, instructive and visual.
Design interfaces need to be minimalistic, instructive and visual.
Offering incentives for content consumption, sharing, and specific health-related behaviors can help nudge users toward desired health-related behaviors. Examples can include progress bars that illustrate levels of content consumption, virtual badges of completion of specific milestones, and associating inadequate engagement as the loss of an award. Getting the right balance of perceived awards and losses motivates users to engage with content that could drive meaningful behavior change.
Technology: Technically, mobile apps need to be light and fast, have low memory and data requirements, and be able to run on slow and patchy networks. Low-income users fastidiously ration their use of data. Transparently displaying their data consumption at every stage can help them make informed choices. The ability to view content offline and share content within their community is also important for engagement.
Design team structure: Multidisciplinary teams that bring together expertise in technology, design, business and sustainability, end-user thinking, and behavioral sciences tend to create the most effective designs. To design for the end user, providers must design with the end user, particularly for populations who are not digitally fluent. Designing with the user translates to understanding their needs and digital behaviors, incorporating their qualitative feedback and behavioral responses at every stage of product development. It’s also important that teams develop a thinking environment and processes that allow for hypothesis development, application design, testing, analytics, and retesting in rapid, parallel, iterative cycles. This allows generation of continual research insights that can guide the product in the right direction.
India and many other countries are increasingly lowering cost and infrastructure barriers for smartphone ownership. It’s now essential to begin planning for health care via mobile applications in the hands of low-income consumers. The success of these applications will be linked to providers’ ability to design content experiences and user journeys that are rooted in local ecosystems, and tailored to the users’ unique conditions and sensibilities. Holistic, multi-disciplinary, iterative approaches will help deliver the complete value of digital tools for inclusive health care.
Read more stories by Alice Lin Fabiano, Aakash Ganju, Sumiti Saharan & Lily W. Lee.


