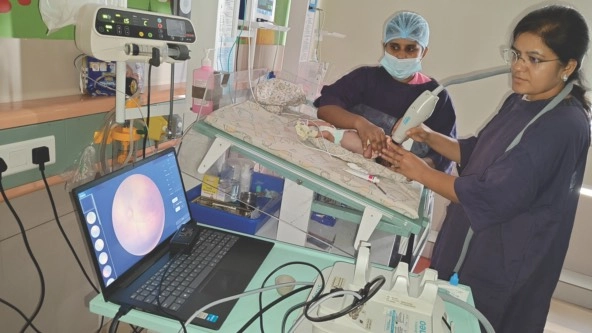
 Dr. Rekha Singhal screens a baby for retinopathy of prematurity in Surat, India, in April 2020. (Photo courtesy of Rekha Singhal)
Dr. Rekha Singhal screens a baby for retinopathy of prematurity in Surat, India, in April 2020. (Photo courtesy of Rekha Singhal)
In April 2018, Qadeer Ahmed’s son, Mohammad Khalid, was born 12 weeks prematurely and admitted to the neonatal intensive care unit (NICU) of a private hospital in Kalaburagi, a city in India’s state of Karnataka. During his nearly two-month stay, a medical team monitored his oxygen levels and treated him for jaundice and blood infections. Mohammad Khalid was also showing signs of developing retinopathy of prematurity (RoP), a disease that occurs in premature infants who are born without fully developed retina blood vessels, which can cause the retina to detach from the back of the eye and lead to blindness.
India has fewer than 24,000 ophthalmologists, with only a little more than 200 trained in RoP. Because neither RoP diagnosis nor treatment was available at the hospital or elsewhere in the city, the pediatrician referred the infant to Karnataka Internet Assisted Diagnosis of Retinopathy of Prematurity (KIDROP), India’s first and the world’s largest telemedicine screening network for RoP.
Each weekday, a two-member KIDROP team—consisting of an imager and a project manager—conducts screenings of premature infants for RoP disease across 31 districts in Karnataka. Six outreach teams visit government-run and select private NICUs—177 in all—in remote areas.
Mohammed Khalid was 48 days old when a KIDROP screening detected that he had in fact begun to develop the disease.
“Nearly 25 percent to 40 percent of premature babies have a risk of developing RoP,” explains pediatric ophthalmologist and KIDROP founder Anand Vinekar, MD. RoP has five stages, and until the second stage of the disease, no treatment is required, since the disease resolves on its own in many infants. But once the disease crosses stage two, the window for successful treatment is short, just 48 to 72 hours. Treating at stage four may still leave the baby with vision loss, and complete blindness can occur by stage five. Therefore, if left untreated, RoP can lead to irreversible blindness.
“Timely RoP screening within the first month of birth is critical because the disease spreads rapidly and is the leading cause of preventable infant blindness across the world,” Vinekar says. The screening program is particularly important in India, which has the most preterm births globally, with blindness affecting 8 in every 10,000 children.
Mohammad Khalid underwent weekly screenings until the disease advanced beyond stage two. Then KIDROP’s screening team advised Ahmed to seek treatment for his son from an RoP specialist within 48 hours. Ahmed’s son went to Bengaluru, Karnataka’s capital city, for laser surgery on both eyes at Narayana Nethralaya Eye Hospital, home to KIDROP’s treatment team of RoP specialists, Vinekar and Snehal Bavaskar. The procedure was a success.
“I’m very grateful to the KIDROP team for saving my son from blindness,” Ahmed says.
Mohammad Khalid is 1 of more than 5,000 babies who have been successfully treated by KIDROP. So far, the program has screened 90,000 infants over more than 300,000 imaging sessions.
A Task-Shifting Model
Vinekar’s interest in RoP began in the 1990s while he watched senior colleagues save infants from blindness during his undergraduate studies in Bengaluru. “It was intriguing to see my seniors look into such a small eye, make a diagnosis, treat the infant, and prevent them from going blind,” he recalls. From 2004 to 2007, he managed the RoP clinic of the Postgraduate Institute of Medical Education and Research (PGIMER) in Chandigarh, North India, where he screened and treated thousands of children.
Vinekar joined Narayana Nethralaya in September 2007 with the intention of creating an outreach program for screening babies for RoP in remote areas of Karnataka.
“At that time—and even now in most states—there was nothing in terms of organized programs for RoP screening,” he says. “Only a few big medical colleges and NICUs in Karnataka were screening, though without proper technology.”
The RoP screening procedure lasts just two to three minutes after a baby’s eyes are dilated.
At the time, babies referred to Vinekar for treatment would come to him with advanced stages of the disease. “Instead of preventing their blindness, I could only offer them rehabilitation options,” he laments.
Understanding both the significant need for screening and the paucity of retina specialists, Vinekar created a task-shifting model, in which a specialist physician’s work is distributed to nonphysicians in under-resourced health-care facilities. Vinekar trained imaging technicians at Narayana Nethralaya to screen infants for RoP, using portable, wide-field imaging cameras (RetCam Shuttles), which can take high-quality images of the retina for accurate diagnosis.
From February 2008 to June 2009, Vinekar ran a KIDROP outreach pilot, sponsored by Narayana Nethralaya, in private NICUs in Bengaluru. In early 2010, the National Rural Health Mission (NRHM) joined KIDROP in a public-private partnership, which targeted six of Northern Karnataka’s most underserved districts in RoP care. Over the next four years, NRHM supported the expansion of the program to 19 districts by providing funding for two screening cameras, a laser machine for treatment, and technician salaries.
Then-NRHM head S. Selva Kumar says he was immediately drawn to Vinekar’s passion for curing the disease. “At that time, we were looking for ways to prevent blindness in the region, so when Dr. Vinekar approached us, we thought it would be a win-win situation for both of us,” Kumar says.
While the partnership’s contract extends through 2027, NRHM no longer provides financial support to KIDROP, since Narayana Nethralaya committed to fully funding the program beginning in 2014. To help cover organizational and services costs, the program charges private hospitals a fee of Rs. 300 to 750 ($3.50 to $8.50), depending on whether it is a corporate or charitable hospital. KIDROP offers free treatment at government-run hospitals.
In India, where 65 percent of the population lives in rural areas with limited health-care access, KIDROP’s task-shifting model plays a vital role in serving underserved regions.
Its outreach team, composed of an imager and a project manager, visits remote hospitals where parents are present with their infants. The team screens both premature babies still admitted to the NICU and those recently discharged.
The screening procedure lasts just two to three minutes after a baby’s eyes are dilated. Keeping the baby comfortable in a swaddle, the imager fits a speculum on the baby’s eyes to keep them open and lubricates them with an anesthetic. The imager then takes photos of the retina and optic nerve and uploads the images to KIDROP’s telemedicine platform, where, in three to four minutes, an ophthalmologist analyzes them and sends a diagnosis to the imager, who shares that information with the parents.
If an ophthalmologist confirms RoP in an infant, the parents are asked to schedule weekly appointments to track the advancement of the disease. Ensuring that parents return for follow-ups, however, can be challenging. It’s easier to treat babies still in the NICU—discharged infants often require parents to travel long distances for consultations, navigating buses and auto-rickshaws with their newborn.
Scaling Through Tech Innovations
Seeking a more affordable camera to expand the program’s outreach, Vinekar collaborated with the Bengaluru-based medical technology company Forus Health in 2012 to develop the 3nethra neo, a camera priced at one-tenth the cost of a RetCam Shuttle. Vinekar says that 3nethra neo is more affordable, is more easily portable (it fits into a briefcase), and has a better resolution and illumination than the RetCam.
In 2013, Vinekar worked with the Indian government to introduce universal eye screenings for all newborns up to 1 year of age through the public health-care system. Despite these guidelines, compliance was limited due to the lack of a legal mandate. In 2015, RoP screening became mandated by law as part of essential newborn care provided by the government.
A shortage of RoP specialists and the high cost of technology to support telemedicine limit screening and treatment of RoP. Even at Rs. 1.5 million ($17,923), the 3nethra neo remains expensive, and hospitals often prioritize incubators and other lifesaving natal equipment.
Vinekar is actively working to overcome barriers in RoP care by expanding the pool of trained professionals. Narayana Nethralaya offers two- to four-week screening training for any interested professional and a four-week RoP fellowship for ophthalmologists. Since 2009, more than 50 ophthalmologists and more than 100 nonmedical imagers have been trained to conduct screenings. KIDROP also plans to incorporate artificial intelligence to triage retinal images, which can then be verified by imagers.
With financial assistance provided by Have a Heart Foundation beginning in 2022, KIDROP has expanded to eight states. Vinekar’s task-shifting outreach model has been adopted by nine Indian states and 13 countries, including Nepal, Mexico, Lebanon, Australia, and Thailand.
RoP specialist Rekha Singhal has replicated the KIDROP model in Gujarat, in western India. During her fellowship at Narayana Nethralaya beginning in 2014, she witnessed how the KIDROP model became established as the standard of care for RoP. When she returned to Gujarat and resumed her medical practice in 2019, she found that babies were losing their sight because of low awareness of RoP among pediatricians and a lack of specialists for treatment. “Parents, even in the city, weren’t aware of RoP, and doctors didn’t inform them,” she says. Many babies referred to her for laser surgery were already in the advanced stages of the disease.
That year, she bought a 3nethra neo camera, trained a technician for screening, and started screening outreach in Surat, in southern Gujarat. KIDROP gave her advanced training and helped her imager get accreditation. Today, her outreach covers underserved areas within a 350-mile radius of Surat, including 18 NICUs where screening and treatment are provided free of cost with financial support from Have a Heart Foundation.
In the next decade, KIDROP aims to expand to all of India’s 28 states and eight union territories.
Read more stories by Priti Salian.


