Imagine for a moment that the United Nations Security Council held its meetings without the use of translators. Imagine leaders from various countries trying to solve challenging problems without understanding clearly what the others are saying. How effective would they be? Isn’t it likely that there would be major misunderstandings that could lead to serious consequences? While this scenario is laughable, many organizations face a similar scenario when they attempt to collaborate with organizations from other sectors—namely the corporate, nonprofit, and government sectors. While cross-sector collaboration is central to solving the complex, “wicked” problems of our times, each sector is unique and has its own way of approaching problems. Without a common language (or a translator), this can lead to stilted progress and wasted time even though all parties are working diligently to create sustainable impact. A framework for visualizing complex problems and a common language for talking about them can mean the difference between the successful execution of an innovation strategy and a frustrating, drawn-out program that yields few results.
My recent book, The Social Innovation Imperative, introduces a methodology for establishing a “blueprint” that maps out a problem and a common language for defining unmet needs of the individuals and organizations involved. The approach enables disparate groups to more successfully define and innovate around a common problem; it also provides concrete metrics by which they can measure results. (As an example, I’ll use a newly launched innovation program—frequently referred to as “aging in place”—that focuses on enabling aging adults to maintain their independence as long as possible.) The formula for creating this common language involves six steps, depicted in the illustration below.
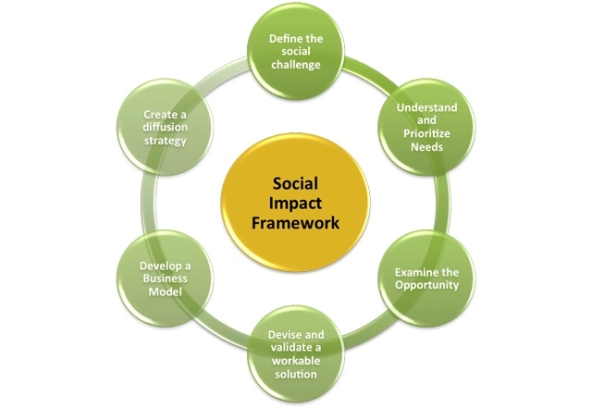 A six-step methodology.
A six-step methodology.
The first three steps form the foundation needed to create a common language for innovation:
1. Untangle the problem. Start by dissecting the problem: Identify stakeholders, context, and potential constraints (both environmental and human). The output of this important step is what I call an “innovation blueprint”—all participating organizations contribute to it, and it ensures a shared view of the problem. The blueprint below shows the context for an innovation program that helps seniors live independently in their homes, avoiding costly nursing home care.
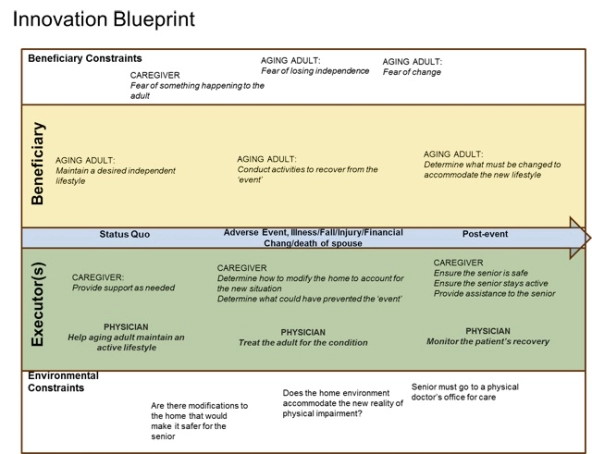 An Innovation Blueprint for aging in place.
An Innovation Blueprint for aging in place.
2. Identify and prioritize needs. What are the needs of the stakeholders—that is, what are the very specific, actionable “jobs” they are trying to do and what is getting in the way of achieving them? The output of this step is a statistically validated, prioritized set of needs for all stakeholders. By identifying the overlap, or synergy, between the needs of all parties, as well as any conflicting needs, innovation efforts become focused and optimized. The diagram below illustrates a handful of synergistic and conflicting aging-in-place needs of seniors, caregivers, and physicians. At the intersection of these three groups, we find that they want to ensure coordination of care among physicians and specialists, know when to seek medical attention, and improve the physical health of the senior. However, they are also in conflict: Seniors’ don’t want to feel “checked up on,” and caregivers and physicians want to know whether the senior is truly adhering to the treatment plan.
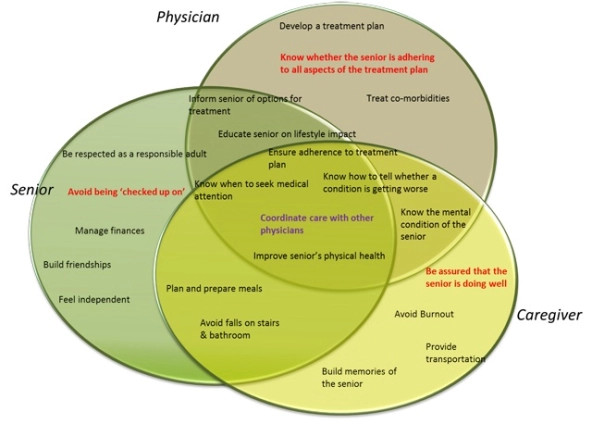 Finding synergies and resolving conflict for aging in place is central to creating innovative solutions.
Finding synergies and resolving conflict for aging in place is central to creating innovative solutions.
3. Understand why. Once you’ve identified and prioritized the needs of each stakeholder, work to gain a deeper understanding of what is preventing them from getting their jobs done—both from their perspective and relative to the overall environment and industry (for example, policy or procedural barriers, or access issues). In many cases, the biggest issue is that the organizations working to solve the problem are not aware of the top unmet needs they need to address.
In the example above, one of the issues that both caregivers and seniors find on the job of “coordinate care” is difficulty knowing what they are responsible for communicating—for example, what they need to tell the physician versus what is in the medical records. Internally, an important issue that health care providers must examine is that there is no “captain of the ship” when it comes to coordinating care for a senior with multiple medical issues.
By understanding a) that there is a big issue for all three groups and b) why it is an issue, developing solutions becomes a much more straightforward task—not necessarily an easy one, but certainly more straightforward.
Cross-sector collaboration isn’t easy, but armed with a common vision and a process for creating a common language (your translator), everyone involved can spend less time on misunderstandings and more time on creating lasting change.
Read more stories by Sandra Bates.


