When Gary Lockley climbed into his car on a July afternoon in 2018, he was feeling relaxed. The sun was shining, and he judged by the traffic that the drive to work would take less than five minutes. Yet, what began as an uneventful day ended with Lockley
in a hospital resuscitation unit by the bedside of a woman saying to him, “Thank you for saving my life.”
“I was sitting at the traffic light, listening to music, when I thought, ‘What’s that noise cutting in over my speakers?’” Lockley recalls. “Then I realized it was a siren tone, and it was coming from my phone.” Minutes later he was kneeling in the front room of a nearby bungalow giving coronary pulmonary resuscitation and defibrillation to a woman he didn’t know while her husband looked on in distress.
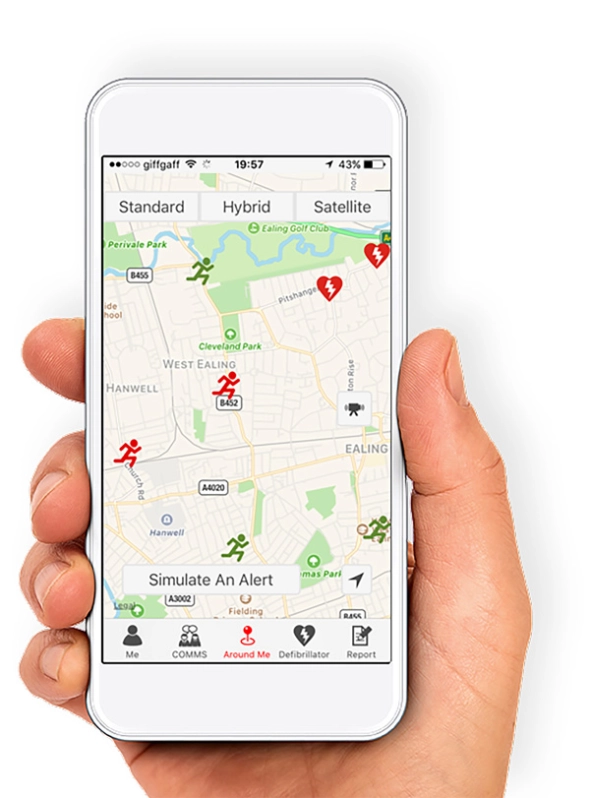 GoodSAM, the world's most advanced emergency services mobile technology platform, maps the proximity of lifesavers. (Photograph courtesy of GoodSAM)
GoodSAM, the world's most advanced emergency services mobile technology platform, maps the proximity of lifesavers. (Photograph courtesy of GoodSAM)
A duty manager in the control room of East Midlands Ambulance Service, part of the UK’s National Health Service (NHS), Lockley is just one member of a growing community of off-duty doctors, nurses, paramedics, and qualified first aiders to use GoodSAM, an app that alerts them when someone nearby has a life-threatening medical crisis. Short for Smartphone Activated Medics, GoodSAM is the brainchild of Mark Wilson, a consultant neurosurgeon with Imperial College Healthcare NHS Trust in London and an air ambulance doctor. Wilson came up with the idea of using smartphone tracking capabilities to mobilize a volunteer community and shrink the delay in response time when emergency services are called to the patient receiving basic life support. “With our air ambulance work, though we get to patients very quickly, often we find patients have suffered brain injuries or even died in the few minutes before we arrive.” This experience is not unusual; mere seconds can determine life or death. “If you look at cardiac arrest survival on the streets of London, it’s about 9 percent,” Wilson says. “But at Heathrow Airport around 80 percent survive, and the reason they survive is that there’s an AED defibrillator at every other gate, and all air crew are trained in basic life support.”
Numbering some 25,000 UK responders as of September 2018, GoodSAM is fulfilling Wilson’s vision of harnessing mobile technology and first aid skills from within the community to save lives. Just a kernel of an idea in 2013, the app is now available in three of the 14 regional ambulance services in the United Kingdom and is in the process of integrating with an additional five. It is also expanding internationally, taking its volunteer network to more than 40,000 worldwide.
A Value-Added Tool
To turn his idea into reality required both technology and expertise that Wilson lacked. Through his university role, Wilson met Ali Ghorbangholi, a 21-year-old graduate student with a reputation as a programming ace. Though about to start work as a software engineer at Morgan Stanley, Ghorbangholi agreed to cofound GoodSAM and develop the app as a side project. “I saw GoodSAM as an opportunity to add to my skills and loved that I was building something new that could help people and even save lives,” Ghorbangholi says.
GoodSAM was initially designed as an app to call emergency services and at the same time alert a volunteer community of off-duty medics and qualified first aiders that someone close by needed urgent medical attention. However, this model depended on members of the public already having downloaded the app to their phone, which limited the number of patients. So, in 2014, the cofounders contacted the NHS’s regional ambulance services about integrating GoodSAM into the normal ambulance process for attending cardiac arrests. They continued to recruit a community of volunteer responders and promote the app through social media channels. “For the first few years, we had [no technological integration] with the NHS,” says Ghorbangholi. “But, when the ambulance services saw how good the functionality was and that there was a pool of people ready to volunteer, it became much easier to get them around the table.”
Securing two rounds of grants from the UK innovation foundation Nesta in 2013 and 2016 provided the funding to begin integrating GoodSAM into ambulance services. Neil White, a transformation delivery manager at East Midlands Ambulance Service, learned about GoodSAM at a conference and pushed for its local adoption. The biggest challenge, he recalls, was melding the notion of crowdsourcing skills over a phone-based app with the NHS’s governance-based approach to safeguarding patients through vetting and clinical processes: “Within the NHS, for anyone who provides patient care, we take references and do criminal record checks, while with the principle of crowdsourcing CPR there’s almost a level of trust that the person signing up to the app is both competent and isn’t looking to do harm,” White explains.
GoodSAM has built its technology on three core principles: governance, security, and innovation. To register, volunteer responders must be off-duty doctors, nurses, paramedics, or qualified first aiders trained and assessed to perform CPR by an accredited training provider or charity and verified by identity checks. As an additional safety net, local ambulance services, not GoodSAM, choose whether to alert first aiders from partner organizations, such as the fire service and law enforcement, or to limit the volunteer community to their own staff.
GoodSAM’s emphasis on governance has ensured that the app is not a substitute for the ambulance service, a possibility that would lead to worse outcomes for patients and a loss of public confidence. “Regardless of whether a GoodSAM responder is there or not,” White says, “the ambulance response continues as normal. GoodSAM is only ever a value-added tool, and that is mandated in our dispatch protocol and training.”
Saving Lives
GoodSAM first became available in the London Ambulance Service in 2015, then the East Midlands and North West Ambulance services in 2017. Now when a caller in a partner region contacts emergency services, the control’s computers not only dispatch an ambulance but also alert the nearest GoodSAM responders—and for some patients that makes all the difference. In East Midlands, the average time for a GoodSAM volunteer to reach a cardiac arrest is just 2.5 minutes compared with 8 minutes for an ambulance. Before GoodSAM, says White, just 7 percent of cardiac arrest patients survived the event. Today, that proportion stands at 25 percent.
The ability of GoodSAM to improve survival rates depends in no small measure on the feedback loops linking developers, ambulance crews, and responders. The system is designed to search for the next-nearest volunteer when a responder is unable or declines to respond. “In the early stages, we set the radius at 800 meters and found that was disincentivizing [responders] because it’s too far to travel,” White says. “So, we changed the radius to 500 meters and looked at the types of alerts that we send through, and now [thanks to these and other tweaks] the acceptance rate sits around 75 percent compared with around 30 percent previously.”
The technology continues to evolve to better serve the needs of responders and GoodSAM’s ambulance partners. When GoodSAM launched, it lacked the capability to bypass the silent function on phones (which negatively affected response, as there are circumstances where a volunteer might bar general notifications). So the team worked with Apple and Google to make GoodSAM the first-ever app to give users the option of overriding silent mode. GoodSAM has also worked with its volunteer community to map the locations of public-access AED defibrillators, enabling responders to see the location of the nearest AEDs. It has also developed some enhanced technologies—including a video-streaming facility that emergency services can activate on the caller’s phone to assess the patient’s condition remotely—which it plans to sell to organizations that can afford to pay, and provide to smaller charities for free.
GoodSAM has global ambitions. As of late 2018, it has forged ambulance service partnerships in the United Kingdom, New Zealand, the states of New South Wales and Victoria in Australia, and fire and rescue services in parts of Brazil, with plans for a launch in the United States. GoodSAM’s only external finance is its grant funding from Nesta; it does not rule out taking on investors, but this is not a priority. “We have pretty much managed to grow GoodSAM organically by investing our own money, which is why we both work two jobs, and the advantage is that we’re not bound to investors or obliged to make more money than GoodSAM needs to be sustainable,” says Ghorbangholi.
Michael Ray, a project manager at Ambulance Victoria, says the combination of clinical commitment and pioneering tech sets GoodSAM apart: “We’re partnering with a medical company with great tech that’s passionate about improving cardiac arrest outcomes, as opposed to a tech company doing something medical,” Ray says.
Even so, with each additional client the pressures intensify. “Like every startup, GoodSAM has now reached a point where the founders and the people around them are working 24/7, and the organization needs to move to the next phase,” says Halima Khan, executive director of Nesta’s Health Lab. “As a funder, our role is to support the leadership to build up their team and identify where the skills gap lies.” According to Wilson, that process of adaptation is likely to combine an element of hiring more people such as IT experts, and country project leads and business development specialists to support its expansion.
Building a sustainable business model is another priority. To this end, GoodSAM has established a separate commercial arm, Instant.help, to manage the enhanced technologies that it is developing and use the revenues to provide the volunteer-based cardiac response side of the business, which does not pursue profit, free or cheaply. In the United Kingdom, GoodSAM donates the technology that utilizes volunteers to attend cardiac arrests to NHS ambulance services, charging only a modest fee to cover integration costs. In developing markets, such as Brazil, it is completely free. “This isn’t something that we’re doing for [commercial] benefit; we’re doing what’s right, and the right thing is to save as many lives as possible,” Wilson says.
While still in its early days, GoodSAM is making strides, forging partnerships, and building a global volunteer community prepared to intervene during moments of great need. That’s important, says Lockley, whatever the outcome: “For the family, there’s a comfort in knowing that everything that could be done for their loved one was done,” he says. “For myself, if I make a difference to one person’s life, then I genuinely feel that I’ve changed the world.”
Read more stories by Alicia Clegg.


