On a chilly November morning in North Wilkesboro, N.C., a town of 4,266 in the foothills of the Blue Ridge Mountains, I sit with two young women at the town’s opioid-addiction treatment clinic.
The previous month, President Donald Trump had declared the opioid crisis a public health emergency, six years after the U.S. Centers for Disease Control and Prevention formally declared an opioid epidemic. Since 1999, more than 200,000 Americans have died from prescription opioid overdoses, leading many in the media to compare the crisis to the height of the AIDS epidemic.
The two women, Amanda and Danielle, are meeting with Brooke Stanley, a peer counselor. The pair have been off oxycodone (or “roxies”) for half a year. They live in a two-bedroom apartment with their three kids. Amanda is looking for work, and Danielle takes care of the children. Brooke tells Amanda that she saw a job opening at a diner close to their house and encourages her to apply. Brooke then gently probes them about how they’re doing.
“For the first time in my life, I have a spatula and spoons!” exclaims Amanda, a tall, thin blonde with short hair tucked under a black beanie. She slouches in a gray hoodie with “Appalachian” written across the front.
“And I didn’t have to scrub any burn marks off any spoons!” interjects Danielle.
Being the proud owners of kitchenware without burn marks is not a small victory. Danielle, who describes her childhood as “tough,” has been shooting up for a decade. “I was raised a Jehovah’s Witness, and right after I got out, I got into drugs,” she says.
Half a year into their three-year relationship, Danielle developed an infection from using dirty needles and ended up in the hospital with septic ruptures up and down her arms. When the infection spread, doctors had to cut out a large chunk of her lung. When she woke up, she injected drugs into her IV, which confounded doctors, so she got sent home, where Amanda found her half-dead. “By that point, I weighed less than 100 pounds,” Danielle says. “And we still went back to the drugs, after they took a third of my lung.”
Thanks to Stanley’s tireless work, the methadone that Danielle and Amanda get at the clinic, and their own pluck and resolve, they’ve stayed off of black market drugs so far. When Amanda’s ex-boyfriend tried, once again, to get her back by giving her some roxies, Amanda held on to them for a night, not sure whether to take them, tell Danielle, or throw them out. She ended up flushing them down the toilet.
Stanley—who herself had struggled with opioid addiction—knows how hard it is to stop using and how far they’ve come. “Now they’re sitting in their beautiful apartment, with their beautiful children,” she says. “When I’d gone to visit them, they’d just finished up making play dough. And so it was just a big difference.”
In a place where crime, addiction, and poverty are so intertwined, getting someone on methadone instead of black market pills they might cook down and shoot up is essential. It’s also just the start. Even the everyday activities and luxuries many people take for granted—like, say, having a car to drive to their job—can be out of reach for people who have struggled with addiction for years.
Stanley works for Project Lazarus, a small, innovative nonprofit devoted to preventing overdose deaths from opioids and helping addicts get their lives back. Since its inception in 2007, the organization has worked with medical professionals, law enforcement, schools, and researchers to achieve the seemingly impossible: bringing harm-reduction policies one might associate with Canada or the Netherlands to a conservative Southern county. While critics question whether such policies exert an immoral influence on the addicted, its leaders claim a deeply moral purpose that is grounded in Christian compassion and ambitious enough to help turn around a national health crisis and save countless lives.
Collaborating with Industry
“You can’t rehabilitate a dead person,” the organization’s founder and CEO, Fred Wells Brason II, says as we drive through Wilkes County—which, by 2007, had the third-highest per capita overdose death rate among counties in the nation. Brason is a nondenominational Christian chaplain and a rapid-fire talker with a shock of white hair and bright blue eyes. The organization’s name comes from a story in the Gospel of John, in which Lazarus, one of Jesus’ followers, dies and is raised from the dead by him.
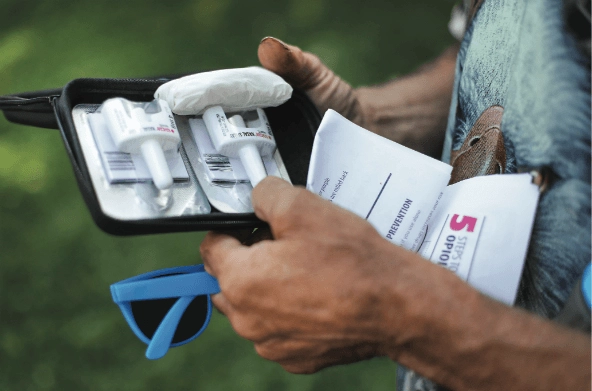 Project Lazarus promotes the
distribution of naloxone kits like
this one to opioid addicts to prevent overdose deaths. (Photo by Richard Lautens via Getty Images)
Project Lazarus promotes the
distribution of naloxone kits like
this one to opioid addicts to prevent overdose deaths. (Photo by Richard Lautens via Getty Images)
But while Jesus’ work was a miracle, Project Lazarus depends on naloxone, a drug that swiftly reverses the deadly effects of an opioid overdose. If administered in time, the drug binds to the same brain receptors engaged by heroin or opioid pain pills. It jolts the user awake, reversing their high and throwing them straight into withdrawal. It’s an unpleasant experience for the user, but it saves lives—if it is administered in time.
But not everyone has the steady hand of a trained emergency medical technician. And for a first responder to show up, someone has to witness and correctly identify an opioid overdose, call 911, and wait for an ambulance to come. What if a child finds a parent passed out and is worried about getting him or her in trouble with the cops? The notifier also has to trust police enough that he or she doesn’t hesitate to call the authorities for help. What if a fellow addict notices an overdose in progress but is scared that he or she will go to jail or lose access to public housing?
“In an opioid emergency … SECONDS COUNT,” notes a website for Evzio, the producer of an injector for naloxone that is so easy to use, even a child could administer it. The device talks the user through the process. “This trainer … contains no needle … or drug,” a Siri-like voice says. “If you are ready to use … pull off the red safety guard. To inject, place black end against outer thigh; then press firmly and hold in place for five seconds,” it instructs. “Five … four … three … two … one … injection complete.”
The device doesn’t have a visible needle, so it’s less intimidating to non-medical professionals. And in the politically conservative Southern county, the less a program conjures stereotypes about drug use, such as needles for shooting up, the more likely it will go over well with local lawmakers and authorities.
Project Lazarus’ primary goal is to save the lives of opioid users, with no moral judgments about addiction and what it might drive people to do. One of the organization’s most important, and controversial, projects in their fight to curb overdose deaths in the county has been to make naloxone as widely available as possible. In 2007, Brason and others testified to the North Carolina Medical Board on the lifesaving powers of naloxone. As Brason recalls, board members admitted to being skeptical at first. They quickly changed their minds after seeing the presentation and issued an official statement of support.
“The prevention of drug overdoses is consistent with the board’s statutory mission to protect the people of North Carolina,” it said. “The board therefore encourages its licensees to cooperate with programs like Project Lazarus in their efforts to make naloxone available to persons at risk of suffering opioid drug overdose.”
To realize that vision, Project Lazarus has even partnered with Purdue Pharma—the company that, thanks to its development and marketing of OxyContin, is widely blamed for fueling the opioid epidemic—to provide naloxone to the county’s opioid treatment program, which Project Lazarus helped found, free of charge to patients. The organization has also received grants from drugmakers Zogenix and Kaleo, and Ameritox, a drug-testing company, has also contributed, the Washington Examiner has reported.
It’s no secret that corporations use philanthropy to whitewash past (and present) sins. Is a Faustian bargain worth it if it saves lives?
“We certainly have taken the hits and criticism for such engagement, which keeps us guarded to ensure any relationship is [of] the utmost integrity,” Brason says. “I am a patient advocate, so to ensure all hands on deck to address the entire issue, everyone needs to be at the table,” he says. “In that light, we engaged industry with ‘no strings attached’ and them knowing full well the expectation to reduce opioid prescribing and engage more of the modalities for pain treatment that could be utilized.”
Ultimately, Brason notes, his personality is more suited to diplomacy than confrontation, an approach that shapes the work of the organization. “As long as we see mutual collaboration at the table within industry—seeking only patient care, treatment, safety, and being responsible—we feel comfortable continuing,” he says. “Industry is not going away, so let’s build the right relationships with mutual goals.”
Deaths of Despair
Wilkes County so perfectly embodies the blight of rural America that it has become a prime destination for reporters looking for insight into Appalachian decay. A 2016 New York Times article, set almost entirely in a vape shop, rankled locals who pointed out that the reporter ignored people such as the hard-working staff of Project Lazarus, devoted to bettering people’s lives. In 2016, PBS also went to Wilkes County to ask, “What do people living in poverty want the presidential candidates to know?”
It’s not hard to see why reporters go there to document American decline. The widely reported 2015 study by economists Anne Case and Angus Deaton, “Rising morbidity and mortality in midlife among white non-Hispanic Americans in the 21st century,” which found that white rural Americans were dying at record rates from “deaths of despair” such as by suicide, drug overdoses, and alcohol poisoning, could have been set in Wilkes County. In 2015, thanks to lowered life expectancy, it ranked in the bottom third in North Carolina for health outcomes, in a state ranked in the bottom third nationwide.
Driving through the forested hills, you catch glimpses of trailer parks, isolated family grave plots, and churches. There are billboards advertising exotic travel and nice jewelry, but those luxuries are more aspirational than realistic for many of the county’s residents. Almost half of Wilkes’ households make less than $30,000 annually, according to a report by the North Carolina Poverty Research Fund. Close to a quarter of Wilkes County residents live below the federal poverty level, $12,060 for individuals and $16,240 for a family of two.
A sign on the side of the road pointing the way to the Tyson chicken-processing plant reflects the true reality. Tyson is the county’s largest employer and one of the few that haven’t gone out of business or left the region. Pulling the bones from raw chicken all day is taxing work, but for many people there aren’t alternatives.
Wilkes County has seen a steep decline in a short time. For much of the 20th century, it boasted thriving textile and furniture industries. Lowe’s Companies home improvement and Lowe’s Foods started in the county, and there are retired older people who live in big houses thanks to the kind of salary people used to make working in corporate for Lowe’s. Much of the manufacturing disappeared in the 1990s. Lowe’s Companies transferred its headquarters to a suburb of Charlotte in 2003.
“In quick succession, a seismic shift occurred in the county, shrinking its economic base to a fraction of what it had long been,” write Gene Nichol and Heather Hunt in “Mountain Poverty and Resilience,” a report published in 2017 by the North Carolina Poverty Research Fund, focused on Wilkes County. “Then the great recession hit,” they write. Median income in Wilkes dropped from $47,992 in 2000 to $33,398 in 2014, a 30 percent decline, according to a report by the Pew Charitable Trust, making Wilkes second in the country for most dramatic income loss. This was yet another reason for the thriving black market in pain pills.
“It’s not surprising our problem is with pain pills,” Brason observes. “They cure pain.”
Brason caught the first glimpses of the opioid crisis in 2004. He was working as a chaplain in hospice care when he noticed that his patients’ pain pills seemed to be disappearing. As a chaplain who’d comforted dying people for years, he was trusted in the community. So he set about trying to find out what was going on.
One terminally ill woman confided that she was funneling her meds to her grandkids so they could sell them to make much-needed money. Many of Brason’s patients said that family members stole their pills, to take or peddle. Opioid painkillers were in such high demand that one dying man was scared to fill his prescription because he thought people would break into his house to steal them. Over the next few years, Wilkes County’s opioid problem exploded, a harbinger of a national crisis. By 2009, people in Wilkes were dying from overdoses at four times the state average.
“When a community is that hard hit—hopelessness, depression, [a lack of] viable opportunities for work—we just have a lot of social determinants that drive substance use, because there’s no other way to cope,” Brason says.
“That’s some people’s source of income here,” Greta Ferguson, a Wilkes County anti-poverty advocate, says about selling pills. “They can go to the pain clinic, get them to trade them off for other people’s food stamps.” According to the sheriff’s office, pills used to go for $1 a milligram. Now it’s $2. That can add up to a lot for people struggling economically, further fueling the market in opioids.
Missionary Zeal
 Project Lazarus founder and CEO
Fred Wells Brason II leads a seminar on his organization’s model at the New College Institute in Martinsville, Va., on March 9, 2016. (Photo courtesy of Piedmont Community Services)
Project Lazarus founder and CEO
Fred Wells Brason II leads a seminar on his organization’s model at the New College Institute in Martinsville, Va., on March 9, 2016. (Photo courtesy of Piedmont Community Services)
Project Lazarus’ offices are attached to Brason’s house. The group has only seven employees. It’s the kind of energetic organization where everyone does a little bit of everything. Program director Donna Parks Hill, for example, recently got certified to teach about addiction in Wilkes County schools. The morning I visited, she was also fielding phone calls from child protective services about a client. “We work closely with the [North Carolina] Department of Social Services, Wilkes County Children’s Services, SAFE [a shelter for victims of domestic and sexual violence], both housing authorities, and many more,” she says.
Project Lazarus’ work is supported by a wide array of partnerships and sources. They’ve received grants from the federal government, state agencies, and private foundations. They also rely on individual donations and contributions from people and businesses in the community. “The philosophy has always been to bring everyone to the table, as all need to be part of the solution,” Brason says.
The organization has partnered with the Mountain Area Health Education Center (MAHEC), recipients of federal funding through the US Centers for Medicare & Medicaid Services. They’ve worked with Community Care of North Carolina (CCNC), a nonprofit that seeks to improve health care in the state—they, in turn, are partly funded by the Kate B. Reynolds Charitable Trust. The funding that Project Lazarus gets from CCNC is matched by the North Carolina Office of Rural Health, a state agency. Brason was also a 2012 recipient of a $105,000 grant from the Robert Wood Johnson Foundation.
Tax filings for Project Lazarus in 2016 show that they received $432,258 in contributions and grants, up from $376,291 the prior year. In a region buffeted by economic crisis and high rates of mental illness, Brason and the rest of the Project Lazarus staff have their work cut out for them.
Brason seems up to the task. He has devoted much of his life to missionary work, including stints at orphanages in Mexico. He helped build a high school on an island in Belize. He and his wife, Karen, spent five years in the late 1990s in Northern Ireland. So he accepts a very low ratio of hand wringing to problem solving in any given crisis.
“You get one meeting to complain about a problem,” he says. “Then every meeting after that should be about solutions.”
When Brason first realized the severity of the opioid epidemic in Wilkes County, he looked around to see what treatment was available. There wasn’t any. So in 2009, he collaborated with Mountain Health Solutions, an Asheville-based opioid treatment program, to bring a medication-assisted treatment (MAT) clinic to Wilkes. Today, more than 600 people circulate through the North Wilkesboro Comprehensive Treatment Center, which now dispenses methadone or Subutex, a brand of buprenorphine, depending on patient need.
Methadone, an opioid, prevents the symptoms of withdrawal, and with far more muted effects of a high—it’s harder to fatally overdose on methadone alone. Yet, in a twist that aptly illustrates the complexity of the opioid crisis, if a person taking methadone suffers a relapse, he is more likely to overdose if he piles on other opioids. This is one of the many reasons why Project Lazarus continues to promote wide distribution of naloxone, the drug that revives a person having an opioid overdose. Subutex is a partial opioid antagonist—it blocks opioids by attaching to the same receptors without activating them. It prevents withdrawal symptoms and reduces cravings for opioids like black-market painkillers or heroin.
At 7:30 on a Wednesday morning, most of the 50 seats in the treatment center’s waiting area are filled, in some cases by multiple generations of the same family. There’s a semi-messy children’s play area in one corner, outfitted with Legos and brightly colored chairs.
Clinic director MeLane Childress Barber underscores how much the once-controversial facility has gained acceptance in the community, thanks to the work of Project Lazarus. “The other day, a church asked me about the best time to come bring biscuits to people waiting to get treatment,” Barber says. Cops used to stalk clients at the clinic for easy arrests, but after a few toured the facility and learned more about the work done there, they seemed more openminded, Barber says. Probation officers, tired of having people on their rolls die from overdoses, are starting to come around as well.
Barber describes her job as emotionally draining but “never boring.” And seeing results day in and day out has made her a firm believer in harm-reduction principles, which support the provision of resources to ongoing addicts, such as medication and clean needles, with the goal of treating them and minimizing the harm their addiction may cause. “A harm-reduction approach focuses on strategies that have proven effective at reducing overdose and other harms that can flow from drug use, as well as harms that flow from ineffective drug policies themselves, such as mass criminalization,” says Maria McFarland Sánchez-Moreno, executive director of the advocacy group Drug Policy Alliance.
“We are in a period where we’ve got to embrace harm reduction,” Barber says. “When people say, well, you’re trading one drug for another … or, well, even if you’ve got somebody who’s not doing well. … Are they using less? That’s harm reduction. But we tend to think about this differently than a lot of people in town.”
The clinic’s doctor, Jana Burson, started out as a harm-reduction skeptic. “I was tricked!” the petite brunette half-jokes, recalling that she got into addiction treatment covering for a doctor at a methadone clinic when he went on vacation. “I would tell the patients stupid things, like, why are you on this? When will you get off it?” she says. “Then I saw the changes that happened in these patients, and I thought, there’s something to this. You see someone on their first day, they look like they’d been drug through a hedge backwards,” she says. “Then you see them get a little bit of color in their face. Then they say, I found a job. Another month and they buy a new truck. I never saw those changes in primary care. I never saw diabetics get better; I never saw my hypertensives get better. But here, people actually improve,” she says.
Project Lazarus staffers also work closely with the clinic to help people struggling with opioids to get their lives together. That might include anything from securing custody of their kids to providing them with a gas card so they can drive to get treatment. Staffers set up pill drop-off at the sheriff’s office, so that people can dispose of their pain meds safely. And they train doctors in safe prescription practices. That’s crucial, because there are people who need pain meds and aren’t prone to addiction, and they shouldn’t be denied pain relief because of doctors’ concerns about fueling the opioid crisis.
Once you make sure that someone is alive and on the road to better health, you figure out what the person needs and work to help him or her get it. The group’s philosophy is simple and drawn from Brason’s work as a chaplain. “If people are hungry, you feed them. If they need clothes, you clothe them,” Brason says. “If they’re addicted, you help them.”
The Model
Although Project Lazarus was born in Wilkes County, its model for addressing the opioid crisis is designed to be more widely applicable. The ethos of the organization is that all communities have unique resources that can be marshaled to bring evidence-based solutions to address the opioid crisis—and unique challenges. With the help of the Office of Rural Health, CCNC, and the Kate B. Reynolds Charitable Trust, the model has been applied in communities across North Carolina as different as a Cherokee Nation reservation and a military base. The Pennsylvania State Legislature recently passed a bill establishing a Project Lazarus commission to develop better community-based efforts to prevent overdoses.
Project Lazarus conceives of its model as a wheel with a hub of three essential principles: public awareness, coalition action, and data and evaluation. To raise public awareness, the organization’s members work to challenge unhelpful assumptions about opioid addiction. Then they try to inform and inspire different institutions to fulfill their unique roles in finding solutions to the crisis. “What I learned early on was that if the individual or group I was speaking with did not know, or see, how they were part of the problem and could be part of a solution, they were less apt to be engaged,” Brason notes. So the organization emphasizes communicating the following: “Why am I needed? What do I need to know, and what needs to be done?” That could mean anything from a presentation on how to use naloxone to residents of Wilkes County’s small public housing complex, to talking to church groups about how they can support members suffering from addiction, to holding presentations to groups of doctors about how to treat their patients safely.
Project Lazarus saw early success in training medical providers in Wilkes on safer prescribing practices. Using the Project Lazarus Medical Care Provider Toolkit—developed in conjunction with Northwest Community Care Network—they helped medical providers in Wilkes learn how to manage patients’ pain without facilitating addiction. By 2011, the overdose death rate in the county had dropped by 69 percent; and notably, none of the dead that year had gotten their prescriptions in Wilkes.
Educating the public about opioids is no easy task, given the misinformation that continues to swirl in the media. One of Brason’s biggest pet peeves is headlines that talk about “addicted babies.” “Babies can’t be born addicted,” he fumes. While babies can suffer withdrawal symptoms from being exposed to opioids in utero, addiction requires deliberate use despite the harms. Recently, there’d been rumors floating around, fueled by national media and politicians, about naloxone parties (or, in North Carolina, “Project Lazarus parties”). That’s when addicts allegedly get as high as possible, then revive themselves with naloxone. Brason points out how absurd this is.
“Let’s say you’ve spent your last dollar on drugs to get high. The last thing you want to do is go into instant naloxone withdrawal,” he says. “Our focus groups with users clearly indicate no such desire or practice for such a party.”
The second core value in the hub is coalition action. First, highlevel stakeholders in a community must get on board with solving the crisis. “The fundamental point is to get the decision makers from the key sectors involved,” the Project Lazarus website explains. They should hold a forum “designed to share information with the broader community about the issues of prescription medication misuse, diversion, and overdose.” That should be followed by the formation of a steering committee or “a group of liaisons delegated from each sector along with the most active community representatives.” That’s followed by a working coalition. After that comes a community plan of action. “Establishing a community plan generally happens through a series of workshops. Workshops begin by having coalition members divide into groups by sector—such as clinical care, public health, law enforcement, schools, faith community, general public, and local government—with at least one member of the steering committee in each group.”
It sounds complicated, but it’s not. “It’s door-to-door grassroots,” Brason says. “Going where people were already meeting as they normally would and drawing them into coalition membership and participation.” Each community might have different resources to tap into in order to build useful coalitions.
That brings us to the third principle, data and evaluation. In his quest to persuade authorities in Wilkes County and across North Carolina to embrace harm reduction, Brason says, he’s developed a great relationship with numbers. “You learn to love data, because that’s what convinces people,” he says. Project Lazarus guides adherents on how to collect data and gauge the success or failure of different strategies.
Radiating out from Project Lazarus’ core hub are seven spokes that might take different forms, based on community need. These are: community education, provider education, hospital emergency department policies, diversion control, pain-patient support, harm reduction, and addiction treatment.
It might seem strange that harm reduction is a spoke rather than an integral part of the core hub, given that so many of the strategies the group pursues are informed by harm reduction. But harm reduction can emerge only from the community’s prior commitment and understanding. “Ten years ago, the understanding of harm reduction, especially in rural areas, was not known or even understood,” Brason says.
“Obviously, Project Lazarus desires to reduce harm, as evident in every spoke,” he continues. “The spoke started out just to be naloxone, and I changed it to harm reduction to allow for the eventual addressing of all harm reduction modalities: naloxone, syringe exchange, safe injection sites, etc.” This is “revealing the changing landscape of the issue—all aspects are continually in development in order to meet changing needs.”
In Wilkes County, the main problem has historically been with pain medications such as oxycodone. The county’s geographic isolation has prevented heroin and fentanyl from polluting the black market in drugs—so far. So in Wilkes, it makes sense to emphasize diversion control, which involves educating the public about how to safely dispose of their pain meds, so that the drugs don’t end up on the black market. The Project Lazarus mantra regarding pills is, “Take Correctly, Store Securely, Dispose Properly, Never Share.” They’ve promoted these core concepts through a community tool kit (funded in part by Purdue Pharma and in part by the Mountain Area Health Education Center). The tool kit is designed to be shared as widely as possible: in town hall meetings; by way of specialized task forces; in public information campaigns on billboards, the radio, and television; and in presentations at colleges, community forums, churches, and schools.
The campaign is a good example of the positive relationship that can be created between public information and coalition building. In 2013, the message to dispose of pills safely was bolstered when two secure drop boxes came to Wilkes: one in the Wilkes County Sheriff’s office and another in the North Wilkesboro Police department. The photo from the opening shows a group of Wilkes County stakeholders beaming, including Brason; Linda Creek, chairperson for Crime Stoppers; J.L. Chappel, a probation officer; and Sheriff Chris Shew.
While diversion works in a rural area, it might not make sense as a priority in an urban area that’s already been overrun by heroin and fentanyl. Yet, in both contexts, arming as many people as possible with naloxone should still be a priority, since the drug can save the life of a pill addict and a heroin user. If heroin spiked with fentanyl makes inroads in Wilkes, as it has in parts of the country closer to drug smuggling routes, ensuring that potential users and their family members have naloxone on hand should save lives.
It all comes back to the nonprofit’s primary goal: to lower the rate of preventable deaths caused by opioid addiction, whether that’s through giving out naloxone, educating doctors on safe prescription practices, getting someone to the Wilkesboro treatment center, or figuring out how they can cope with the stressors that might drive them to drug use in the first place.
“Everybody dies, but there are good ways and bad ways to die,” Brason says, recalling his time working as a chaplain in hospice care. “You can die well.”
When he counsels older people and their families, it’s a whole different process than when a young person drops dead from drug use. “Most older people don’t regret what they did. They usually want to restore their relationships with their families. Through death, we restored a lot of families,” he says. “But when a 22-year-old overdoses and dies, the family is devastated. It’s a totally different grieving process.”
 People remember those lost locally to addiction at the Jimi-Jon Jam II concert hosted by Project Lazarus in North Wilkesboro, N.C., on September 30, 2017. (Photo courtesy of Corky Ellis, corkyellis.com)
People remember those lost locally to addiction at the Jimi-Jon Jam II concert hosted by Project Lazarus in North Wilkesboro, N.C., on September 30, 2017. (Photo courtesy of Corky Ellis, corkyellis.com)
It’s not always easy to work with people affected by addiction, but Brason doesn’t expect human beings to be perfect. “You have to meet people in their present condition,” he says. “Not where you wish they were.”
The Sheriff’s Office
Meeting people in their present condition has proved to be difficult. Lawmakers, police, and service providers have resisted harm-reduction policies, such as MAT, because they violate intuitive norms about addiction and personal responsibility.
“Critically, harm reduction does not insist upon complete abstinence, but rather accepts that in any society, some people are going to use drugs, and instead tries to reduce associated harms,” says Drug Policy Alliance’s Sánchez-Moreno. “For some people, who have been taught that the goal of drug policies should be complete abstinence, it can be hard to accept the basic premise of harm reduction: that some level of drug use is going to happen in society, and so we should try to reduce the harms associated with it.”
Let’s take needle exchanges. The best way to help addicts who are not ready to quit may be to give them a clean needle. That might seem like enabling bad behavior. But if they have clean needles, they are less likely to get sepsis and die. It also prevents the transmission of HIV and hepatitis. Parents can then worry less about dirty needles discarded in parks, and law enforcement can rest a little easier about getting pricked by a dirty needle. Studies have consistently shown that injection drug users are even more likely to end up in treatment if they have access to a needle exchange program, because they are more likely to encounter social workers and other professionals who can help them. A 2000 study in Seattle found that injection drug users were five times more likely to enter methadone treatment if they participated in a needle exchange.
Needle exchanges are now legal in North Carolina. But Wilkes County currently doesn’t have one because they remain controversial. Change happens slowly. Tessie Castillo, a North Carolina Harm Reduction Coalition staffer based in Raleigh, says that even though the state as a whole is starting to embrace harm reduction, momentum is stalled by the institutional prerogatives of the criminal justice and medical systems.
“In North Carolina and the United States, we still treat addiction as a criminal justice issue and not a health issue,” she says. “We’re still spending a lot of money on law enforcement, exacerbating the problem. People are embracing the language of public health, but the wheels are turning very slowly. The criminal justice system and the medical system are behemoths and entrenched in the way they’ve been for a long time. Diverting funds from one area to another is extremely difficult.”
Yet Brason, who has excellent relationships with key stakeholders in the community, has slowly won over law enforcement to some facets of harm reduction. The Wilkes County Sheriff’s office is well versed in the deaths of despair documented by the 2015 Deaton-Case study. Almost every single day, someone calls in threatening suicide. “We had one yesterday, the day before, the day before that, I don’t know how many days in a row,” Sheriff Shew says.
Shew also blames rampant crime on addiction rates. “The domestic violence, the assaults … if it wasn’t for them, our crime rate would be really, really low.” He also doesn’t bother hiding his unhappiness about the pointlessness of arresting and releasing the same addicts and dealers over and over. The deputy sheriff adds that the black market in pills is linked to the county’s economic woes. “When you got elderly folks that are selling their pills to make a few dollars…”
Prior to becoming sheriff, Shew worked narcotics for decades and put many dealers behind bars. “But, there was always someone to take their place,” he says. “We can’t arrest our way out of this.”
But even as law enforcement is starting to acknowledge the limits of treating addiction with incarceration, the Wilkes County jail remains filled with addicts. “Sometimes we can’t even get in touch with our clients,” Brason says as we drive past the jail, a low-slung building with a razor-wired outdoors. That’s a very big problem, especially since if people haven’t been doing drugs in jail, they’re much more likely to overdose and die when they get out. A study conducted in Washington state found that people released from prison are 13 times more likely to overdose than the general population in the two weeks after release.
Shew’s bottom line is that his job is to enforce the law. Police aren’t social workers. Still, his work means that he encounters addicted people almost daily, and he doesn’t understand what motivates them. “I’ve spent countless hours talking to these people trying to figure it out,” he says. He describes a young woman who went to jail for breaking into a house to feed her habit. Her friend had just died. “She was shooting up, she got sepsis, and it killed her,” he says. The woman didn’t seem perturbed by her friend’s death. She told the sheriff that she had to do drugs or she’d get sick.
“She got to where she didn’t want to talk anymore, and I said, ‘You just don’t care if you live or die, do you?’” says Shew. “She perked up and looked at me and said, ‘No, I really don’t.’” She was in her early 20s.
Wilkes Relapses
Despite such struggles, the solutions that Project Lazarus has brought to Wilkes County have arguably saved many lives. But the crisis persists. In fact, overdose deaths have climbed since the county’s banner success in 2011, and addicts are still dying in stark numbers.
The data for opioid overdose deaths in Wilkes compared with the rest of the state demonstrates its success as well as the depth of the problem. In 2006, 26.7 percent of deaths in Wilkes County were from opioid-related accidental poisonings, including prescription pills, heroin, and fentanyl, according to the North Carolina medical examiner’s office. That’s as compared with 7.7 percent in the entire state. Between 2006 and 2016, opioid deaths in Wilkes fluctuated, even as deaths in the state ticked up consistently.
For example, opioid fatalities in Wilkes jumped to 30.5 percent of total deaths in 2008 and 37.6 percent in 2009. In 2011, four years after Project Lazarus was founded, they dropped to 11 percent. The drop is likely due to Project Lazarus’ early success in training county medical providers in appropriate prescribing practices. That year, none of the people who died from a fatal opioid overdose had gotten their prescription from a medical care provider in Wilkes.
Yet, that drop wasn’t permanent. Over the next two years, opioid fatalities in the county stubbornly crept back to around 20 percent and thereafter settled into the 30 percent range. Despite the group’s hard work, Wilkes County has consistently shown higher death rates than the rest of the state, which speaks to the complexity of addiction in the county.
There is also the question of what part of Project Lazarus’ model was responsible for the dip in overdose deaths. Nabarun Dasgupta, an epidemiologist at the University of North Carolina at Chapel Hill who consulted with Project Lazarus, completed a study of its approach. He found that medical care provider education helped reduce mortality.
Dasgupta and Brason blame the arrival of heroin for the uptick, although the evidence for this is anecdotal. But both men insist that Project Lazarus’ work is still making a big difference. Without the interventions orchestrated by Project Lazarus, the death toll in Wilkes might be much higher, had it continued on the same trajectory. Asked if the death toll in Wilkes would have been higher without the interventions of Project Lazarus, Dasgupta said, “Easy, the answer is yes.”
“This further validates the necessary interventions and preventions pertaining to the demand side of substance use,” Brason says. “Wilkes has for many years now eradicated most of direct local access to prescription medications which changed the supply side. Unfortunately, the demand in Wilkes and other communities is due to the social determinant factors, such as environment, culture, poverty, trauma, and abuse. I shudder to think where we would be locally if the 600 people were not in direct opioid-addiction treatment.”
Read more stories by Tana Ganeva.


