 At a clinic located in a slum in Delhi, India, a nontraditional health worker uses a fingerprint scanner to register a new tuberculosis patient. (Photo by Andrew Aitchison/In Pictures/Corbis/AP Images)
At a clinic located in a slum in Delhi, India, a nontraditional health worker uses a fingerprint scanner to register a new tuberculosis patient. (Photo by Andrew Aitchison/In Pictures/Corbis/AP Images)
For generations, the model of how people in the developed world access health care services has involved face-to-face encounters between doctors and patients in brick-and-mortar medical facilities. The contours of that model are well known: A patient arrives in a clinic, registers her insurance at the front desk, and waits. Then a nurse or an aide ushers her into a sterile room, takes her vital signs, and hands her a paper gown. Some minutes later, a doctor in a white coat enters the room, asks her questions for 10 minutes or so, and conducts a brief physical examination. The doctor issues a diagnosis, writes a prescription, and sends the patient off to make a copayment. Afterward, the patient will drive to a local pharmacy to purchase medication. She is one of 40 patients whom the doctor will see that day.
In developing countries, that model of access is structurally untenable. According to the World Health Organization, there is a global shortage of 4 million health care providers; in 57 countries, by the WHO’s reckoning, that shortage amounts to a “crisis.” 1,2 The WHO also estimates that 30 percent of the world’s population lacks access to essential medicines.3 Rural clinics in the developing world are scarce and ill supplied, and using better-equipped urban medical facilities often requires patients to make a two-day journey. Even within cities, travel to and from a clinic through jammed streets can take several hours. Urban clinics, moreover, are typically overwhelmed by patient demand. Alternative providers such as local pharmacists are well meaning, but they tend to have limited training. In place of insurance, people must rely on family savings to cover health care expenses. Medications are often counterfeit, serving as placebos at best and causing considerable harm at worst. Across large swaths of the globe, a lack of supporting infrastructure and appropriately trained personnel undermines any hope of replicating the Western model of health care.
But a new breed of innovators who work in startup companies, multinational corporations, NGOs, and government agencies are responding to this challenge by using information and communication technology (ICT) to reinvent health care access. Consider: In a remote area of a developing country, a patient walks not into a medical clinic, but into the home of a local woman. Trained as a health worker, the woman asks a few questions in the patient’s native dialect, takes the patient’s temperature and blood pressure, and then picks up a mobile phone. Within seconds, a paramedic is on the line. Using one of 70 algorithms in a clinical decision-making software package, the paramedic works through another, more targeted series of questions. The local health worker then holds the line as the paramedic, via the Internet, sends a brief summary of the case to a physician for review. The summary includes a diagnosis and a proposed treatment plan. The physician agrees with the diagnosis but suggests a longer course of antibiotics, and signs off. The paramedic comes back on the line to explain the diagnosis and the treatment plan, and the local health worker offers to provide medications directly to the patient. Meanwhile, the physician turns his attention to the next case summary that appears on his screen—one of 400 that he will review that day. That’s not a theoretical scenario. That’s the reality for patients enrolled in eSwasthya, a program offered by the Health Management and Research Institute, a nonprofit organization based in India.
ICT has the potential to topple or at least lower the geographic, financial, and cultural barriers to access that dominate the health care landscape in low-resource environments. Spurred by a rapid diffusion of mobile telephony and by a sharp increase in Internet penetration, many organizations in the developing world are building health programs that hinge on the use of mobile phones, Internet-enabled computers, and other ICT devices. In some cases, these programs complement existing hands-on health care services. In other instances, they present ambitious and innovative alternatives to traditional care.
The new frontier of health care access has many striking features: a radical reinterpretation of what it means to see a health care professional; a redefinition of skill on the front line of care; an amplification of each professional’s productivity; and a vast extension of geographic reach. Yet by far the most significant feature is an intensive focus on the needs of the patient. Programs such as eSwasthya make significant use of ICT, but their primary focus is on providing members of their target population with access to needed care.
The Center for Health Market Innovations (CHMI), based in Washington, has amassed data on 1,200 for-profit and nonprofit health programs.4 The Results for Development Institute launched CHMI in 2010 with funding from the Bill & Melinda Gates Foundation, the Rockefeller Foundation, and UKaid. Since then, the CHMI database has emerged as the world’s leading repository of information on global health innovation. We are all members of the Toronto Health Organization Performance Evaluation (T-HOPE) team, and in that capacity we scoured the CHMI database for programs in the developing world that prominently feature the use of ICT. We focused our attention on programs for which detailed information on organizational strategy and operational results is publicly available. Ultimately, we identified 40 programs that meet those criteria. They cover a wide range of applications—from public outreach on sexual and reproductive health to the use of biometric identification cards in microinsurance plans. But all of them aim to extend and improve health care access.
A Framework of Innovation
To make sense of the many ICT-enabled health programs that have emerged in recent years—and to identify worthwhile candidates for investment or emulation—funders, government officials, and program managers need to have a clear analytical framework. In this article, we introduce a simple yet compelling classification scheme. We believe that the best way to look at innovations in health care access is through the lens of demand: Who will benefit from implementing such programs, and what form will that benefit take? In that spirit, we focus first on the potential users of health technology and then on the uses to which that technology might be put.
Technology is changing what it means to be a user within a health care system. It's changing the range of potential uses as well.
When it comes to ICT-based health access, there are two groups of core users: patients and providers. The first group includes not only patients and their families, but also members of the general population who have an interest in disease prevention and wellness. The second group encompasses a wide variety of health care professionals. This category includes, for example, rural physicians in India who access continuing medical education through Narayana Hrudayalaya, a large hospital chain that delivers training via satellite and fiber-optic technology. But it also includes local entrepreneurs— many of them former tuberculosis patients—who run mini TB clinics under the auspices of Operation ASHA, a program that uses a biometric patient-record system. (Operation ASHA began in India but now operates in Cambodia and Vietnam as well.)
The uses of ICT in health care fall into two broad categories: educating people about healthy living or medical practice, and empowering people to access or deliver treatment. The first use category covers initiatives that aim to increase the knowledge of those who dispense or receive health services. It includes activities that range from issuing SMS bulletins about safe sex to producing online modules that teach new techniques to primary care providers. The second use category involves applications that directly or indirectly affect patient care. It includes (among other uses) telemedicine kiosks, clinical decision-making software, and supply-chain management tools that improve access to medication.
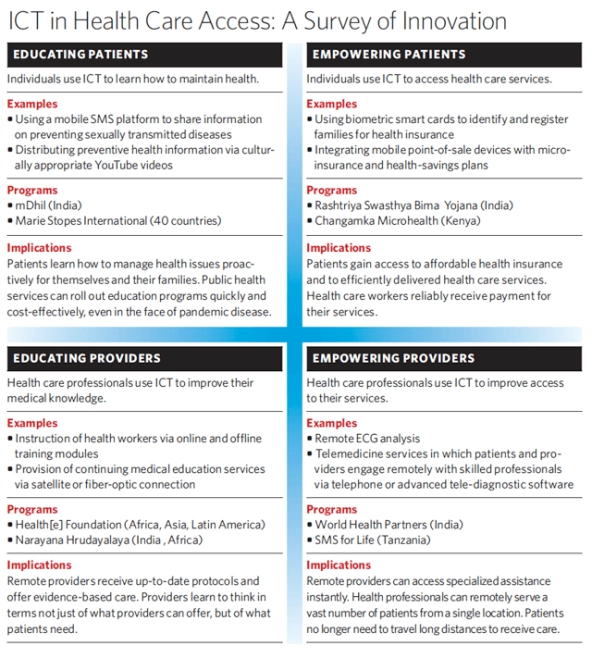
A dual focus on users and uses yields a two-by-two framework that encompasses four broad categories of ICT-based health care innovation. (See “ICT in Health Care Access: A Survey of Innovation,” below.) This framework brings order to the seemingly chaotic landscape of this growing sector. It serves as a map to a fast-changing terrain that will enable decision-makers to evaluate various innovations. ICT is changing what it means to be a user within a system of health care access, and it’s changing the range of potential uses as well. Categorizing and comparing programs from around the world helps us identify where and how that transformation is unfolding globally.
A Survey of the Field
The framework has utility for investors, donors, policy makers, and program managers. For investors and donors, it offers a tool for comparing organizations that apply for funds with peer organizations that target a similar set of users and uses. Similarly, policy makers can deploy the users-and-uses framework to assess public health programming, to allocate scarce resources, and to encourage private investment in a given area. (Many of the examples in the CHMI database represent public-private partnerships, and many others began as private projects that government health departments then took over.) Program managers can categorize their own efforts by referencing the framework. Doing so will help them with strategic planning, and it will also help them to avoid the pitfalls that other organizations have encountered in serving particular user groups or in implementing particular uses.
Now, with this framework in place, we can survey the rich variety of ICT-enabled health programs that populate the CHMI database. (Several of these programs operate in multiple areas of the framework; they serve multiple users and uses. But we categorize them here according to the domain where their impact is especially salient.)
Educating Patients | Two programs in the database offer examples of using ICT to provide accessible health education to the general population.
mDhil, a venture-backed startup based in Bangalore, India, leverages mobile telephony and the Internet to reach its target audience— urban young adults in New Delhi and Mumbai—at a fraction of the cost of traditional education initiatives. In its first year in operation, mDhil attracted 150,000 paid subscribers to its SMS health messaging service. The service costs 5 cents per health tip or 60 cents per month by subscription. Since its founding in 2009, mDhil has aggressively expanded its Internet presence. Its full-featured website covers health issues that range from weight loss to cancer. It also publishes a series of video clips on YouTube that has attracted more than 10 million views. The videos feature recurring personalities who answer questions about various topics; the most popular clips are those that address sexual health concerns. The ability of mDhil to conduct an Internet-based marketing strategy on a large scale distinguishes it from most other programs that aim to broaden health care access.
Marie Stopes International (MSI), based in London, targets men and women in need of sexual health services. MSI has been in operation for more than 30 years, and it currently has centers in 40 countries. Its program in Bolivia, a country with limited communication infrastructure, offers mobile clinic services, finances health care for low-income families, distributes contraceptives, and provides public education on sexual health issues. To promote reproductive health education, MSI Bolivia established a confidential phone line through which adolescents and young adults can ask questions that they find too embarrassing to bring up in a public setting. Trained university students field questions on the line six days a week. If necessary, they refer callers to an MSI clinic for medical care. The cost of each call is about 21 cents, and MSI Bolivia and the caller share the cost equally. MSI plans to expand its service by creating a Web portal for patients and providers, and by enabling patients to book clinic appointments through its confidential hotline.
Educating Providers | The database features two programs that expand access to care by using ICT to improve the training of local health care workers.
Health[e] Foundation, based in Amsterdam, has a simple mission: to deliver state-of-the-art medical information to resource-limited regions of the world. Founded in 2003 by the Dutch physician Fransje van der Waals, Health[e] Foundation offers a blended curriculum that combines brief, periodic on-site training sessions with three-month-long e-learning modules that participants can take online or offline (via USB memory stick). The modules address a broad range of topics, including HIV and AIDS, tuberculosis, and mental health. At the end of each module, participants receive a certificate, along with access to course updates and continuing-education materials. Medical experts from around the world help to create and curate this educational content. Health[e] Foundation operates on every continent except North America and Antarctica, and it presents its course material in multiple languages. Each year, about 1,000 physicians, nurses, and other health workers receive training through the foundation.
Narayana Hrudayalaya, based in Bangalore, India, supplements its core health care services by operating a highly advanced provider education platform. The Narayana facility in Bangalore is one of the world’s premier cardiac surgery centers. It has 5,000 patient beds, and it’s best known for offering a low-cost ($2,000) coronary artery bypass procedure. Recently, Narayana began a less publicized venture into continuing medical education and telemedicine. It joined the PAN African e-Network, a multiorganizational initiative that uses satellite and fiber-optic technology to bring Indian expertise in education and health care to sub-Saharan Africa. Initially, the network focused on providing remote consultations and ECG readings to in-country health care workers. But Narayana, which is leading the health care aspect of the project, quickly recognized the potential of the network to deliver educational content to African physicians. Today, Narayana offers remote educational services in 16 African nations.
Empowering Patients | Several ICT-enabled programs in the database augment the ability of low-income patients to access standard health care services.
Rashtriya Swasthya Bima Yojana (“National Health Insurance Program”), based in India, uses portable biometric data collection and other ICT methods to support a nationwide insurance plan. The program has helped establish affordable access to care for about 34 million poor Indian families. It’s a public-private partnership in which the Indian government serves as the payer, third-party insurers provide risk coverage, and contracted administrators manage enrollment and claims. The federal government covers 75 percent of the cost of premiums, and state governments cover the remaining 25 percent. Each participating family pays a one-time fee of 30 rupees (about 70 cents) at the time of enrollment. The head of each family and four other family members have their fingerprints and picture taken at a terminal that immediately adds them to a central database and generates a chip-enabled smart card. At that point, family members may use the card to access about $600 worth of hospital services. Several features of the plan help patients to avoid delays in care. The authentication, claims, and authorization processes are tied to a patient’s smart card, and they are completely paperless. The plan also offers preapproval and fixed pricing for 750 procedures and claims. To participate in the service, hospitals must have a reliable Internet connection, and they must install fingerprint and smartcard readers. The service closely monitors hospitals for possible fraud and quickly removes offending institutions from the program.
Changamka Microhealth, a Nairobi, Kenya-based insurer that began operation in 2008, also issues smart cards. The organization targets people who have some income but are unable to open a savings account at a traditional financial institution. With a Changamka card, users can visit a doctor or buy medicine at more than 30 accredited establishments in Nairobi, Kikuyu, Mombasa, and Naivasha. Changamka has negotiated discount rates with each of those providers. Patients can use the cards for outpatient treatment, maternity care, third-party payment, or in-house services that their employers provide. The cards are available at supermarkets and other retailers, patients can add money to the cards at a cellular-connected terminal or through a mobile phone, and the cards do not expire. Changamka has partnered with GA Insurance, a Kenya-based company that acts as both underwriter and fund manager for the organization.
Empowering Providers | Finally, several programs in the database deploy ICT systems to enhance provider-side efficiency.
World Health Partners (WHP), based in New Delhi, offers an example of ICT-enabled remote primary care. WHP, a nonprofit partnership, began as an 18-month pilot in the Indian state of Uttar Pradesh, and more recently it has expanded to Bihar, one of India’s poorest states. WHP recruits pharmacists, local health workers, and other informal care providers and sets them up in franchised “clinics” under the WHP brand. The clinics mainly handle primary care complaints, but patients can visit them for preventive medicine, for tuberculosis treatment—or for anything in between. As with eSwasthya, patients first consult a local WHP franchisee and then connect via telephone or videoconference to a remote physician. After the consultation, the physician can send a prescription to the clinic via SMS. WHP maintains laboratories for blood work, X-rays, and ultrasound tests, and it runs WHP-branded pharmacies as well. Patients pay less than $1 per visit, of which 60 percent goes to the franchisee and 40 percent goes to WHP. There are 250 telemedicine centers in the WHP network, and thus far WHP providers have served about 750,000 people. Today, WHP franchisees operate in 4,000 villages in Bihar. But the partnership is adding villages to its network at a pace of 400 per month, and its goal is to serve 20,000 villages by 2015.
SMS for Life, a system for improving supply-chain management, shows that provider-side ICT implementation can go well beyond enabling telemedicine. The project began as a pilot program in Tanzania, a country with endemic malaria. About 93 percent of the population is at risk of malarial infection, and there are an estimated 60,000 deaths annually from this preventable illness. To prevent stock-outs of antimalaria medication (among other crucial supplies), the Tanzanian Ministry of Health and Social Welfare partnered with Novartis, IBM, and several multinational organizations to develop a system for monitoring supply levels across the country. Each Thursday, health facility workers receive an automated text message that asks them to report on their stock levels. If they don’t reply within 24 hours, they receive a reminder message. The next Monday morning, a district officer receives a summary report of supply levels throughout a given region. The officer can then order additional supplies or redistribute supplies from one facility to another. Within six months of the start of the pilot, the stock-out rate in Tanzania declined from 79 percent to 26 percent.
Assessing the Data
Sorting the ICT projects in the CHMI database in accordance with the users-and-uses framework helps shed light on areas of health care where the application of ICT has been fairly robust—and on areas where there are notable opportunities for further innovation. A large number of these projects, for example, focus on empowering either patients or providers. They target populations that traditional services have been unable to reach, and they do so by overcoming limitations related to geography, transportation, and the high cost of delivering on-site services. These examples provide other organizations with models for bringing together traditional and nontraditional providers to enable services that do not require brick-and-mortar facilities or face-to-face interaction.
There are also multiple entries in the CHMI database that fall within the patient education domain. These services, which often rely on cell phone and SMS technology, take advantage of the explosion in mobile telephony that is occurring in even the poorest communities around the world. These services have one other advantage: The organizational infrastructure needed to initiate them is relatively simple.
By contrast, we found notably few examples of ICT-based innovation in the provider education domain. The reason for that gap is twofold, we believe. First, training providers is a highly technical undertaking—considerably more so than, say, launching a mass SMS campaign to teach the general public about condom use. It requires both medical and educational expertise, along with a deep understanding of local provider practices. Second, although many Western medical schools are working with schools and governments in the developing world to improve provider training, the standard approach continues to focus on delivering such assistance on-site and in person.
These barriers are surmountable. We expect to see slow but significant growth in ICT-enabled provider education, especially as ICT infrastructure becomes more prevalent in the developing world and as educational institutions there become more sophisticated. Established schools such as Stanford University and startup ventures such as the Khan Academy (a nonprofit video-based education service) are already demonstrating that educators can conduct large-scale knowledge transfers—even entire university courses—via the Internet. It’s only a matter of time before similar approaches to educating providers begin to take hold in developing countries.
Until recently, program managers with an interest in ICT-enabled strategies to improve health care access had few examples to follow. Fortunately, as the programs in the CHMI database indicate, promising examples are now emerging. The next challenge will be to evaluate the long-term viability and the outcomes of such programs, and that will require looking beyond simple metrics such as the number of people who have been treated or trained. A working group that includes CHMI, T-HOPE, and the Global Impact Investing Network is developing a set of metrics for investors and funders to use in assessing new health care projects. But that effort will take a significant amount of time to unfold. Meanwhile, tools such as the users-and-uses framework help to illuminate the variety and the depth of activity in this emerging field.
Assessing the Future
Numerous limitations continue to affect the implementation of ICT-based health care solutions. Internet connectivity is still nascent in much of the developing world. The instability of electrical supply in developing countries presents a massive challenge as well. And although mobile-phone service is becoming ubiquitous, high rates of illiteracy limit the usability of SMS-based programs in many parts of the globe. In a recent post at SSIR Online, Ken Banks noted that organizations continue to push technology—mobile technology, in particular—into low-resource settings without fully taking into account local needs.5 The use of ICT in health care is still in its infancy, and we shouldn’t let its novelty distract us from the need to assess its relevance to target communities. Health care technology, in short, cannot surmount all barriers to health care access.
Despite those obstacles, there are substantial opportunities to expand ICT-enabled health care services. Most developing countries now have the telecommunications infrastructure to support at least basic ICT services, and those services can readily improve access to health care treatment and education through the deployment of voice and SMS applications. More sophisticated services, meanwhile, are emerging in countries that have both a strong technical infrastructure and a sophisticated organizational infrastructure. Fortunately, more and more countries do have that combination of resources.
We are likely to see rapid growth in demand-focused, technology-enabled services that address the needs of both patients and providers.
What’s more, the potential scalability of ICT-based services offers an opportunity for organizations to extend their programs beyond individual countries. After all, many developing countries suffer from similar gaps in health care access and face similar infrastructure limitations. At least five of the 40 programs that we identified in our survey are transnational in scope. We have already discussed four such programs: Operation ASHA, which sponsors TB clinics in multiple Asian countries; Health[e] Foundation, whose provider education platform reaches physicians in Asia, Africa, and South America; Marie Stopes International, which offers sexual and reproductive health services in 40 different countries; and Narayana, an Indian organization that participates in the PAN African e-Network. In addition, a program called Dentista do Bem coordinates the efforts of volunteer dentists in Portugal and in numerous countries throughout Latin America. Other ICT-enabled approaches—with due allowance for the need to make cultural and linguistic modifications—have the potential to extend across national borders as well.
The innovative programs in the CHMI database reflect a disruptive model of care that has not yet spread from developing countries to more resource-rich settings. The broad use of advanced telemedicine and clever smart-card-enabled insurance schemes are rare or nonexistent in much of the developed world. Yet the potential benefits that those services could bring to the operation of, say, an American HMO (health maintenance organization) or a Canadian LHIN (local health integration network) are immediately apparent. Indeed, given their relative freedom from technical obstacles and their high literacy rates, developed countries present an environment in which ICT-driven health care clearly might flourish. One place to start would be in the use of long-established mobile technologies— an area where “advanced” countries have lagged behind their less-developed counterparts. SMS-based payment and health education applications have become commonplace in many developing countries, for example, even as people in the developed world focus on creating medical smartphone apps that have struggled to find broad utility.
In all parts of the world, the largest barrier to implementing ICT-based health care is not a lack of technology or a lack of medical skill. Instead, it is the belief—prevalent in both the developing world and the developed world—that high-quality health care services require hands-on, person-to-person engagement within a traditional brick-and-mortar medical facility. As that mindset changes and as organizational and logistical capabilities continue to improve, we are likely to see rapid growth in demand-focused, ICT-enabled services that address the needs of both patients and providers. Technology that can improve access to health care now exists, and it’s becoming ever more widely available. We simply need the motivation and the courage to use it.
We wish to thank Ameya Bopardikar, Jieun Cha, Earl D’Almeida, David Leung, Leigh Pharand, and Jason Sukhram for providing research support for this article. We are also grateful for the financial support provided by the Center for Health Market Innovation, the Results for Development Institute, and the Canadian Social Sciences and Humanities Research Council.
Read more stories by Anita M. McGahan, Will Mitchell, The T-HOPE Team & John A. MacDonald.


