 (Illustration by Richard Mia)
(Illustration by Richard Mia)
Today, heart disease, stroke, diabetes, asthma, and other chronic diseases account for about 70 percent of all deaths in the United States and restrict daily living activities for 25 million people.1 They also impose huge costs on families and the economy, gobbling up an estimated 75 percent of the money Americans spend on health care.2 Unless we can reach people at risk of chronic disease with the right interventions, these preventable diseases threaten to halt or even roll back significant gains made in Americans’ health and life expectancy. In fact, some experts predict that if chronic diseases continue to grow at the present rate, children born today will be the first generation in two centuries to live shorter lives than their parents.
In short, the battleground for public health has shifted from infectious to chronic disease. Major infectious diseases of the 20th century, like polio, were brought under control through the development and dissemination of vaccines, but today’s chronic diseases require a different approach. The causes of most chronic diseases are a complex interplay between where we live and how we live. So it stands to reason that tackling these diseases will require interventions focused on both our environments and our lifestyles. Environmental interventions that ban smoking in public places or the use of trans fats in packaged food are necessary but not sufficient. Behavioral interventions that help people quit smoking or eat nutritiously are an equally important part of the equation.
The good news is that for some chronic diseases we have a pretty good idea of what it takes to change individual behaviors. Consider diabetes: 26 million Americans already have the disease and another 79 million are estimated to be at risk with prediabetes, a condition where blood glucose levels are higher than normal but not yet high enough to be diagnosed as diabetes.3 The National Institutes of Health (NIH), the Centers for Disease Control and Prevention (CDC), and others spent more than $200 million over 10 years to study a structured lifestyle intervention that helped people with prediabetes lose 5 to 7 percent of their weight and participate in daily physical activity such as brisk walking. The results were impressive. The Diabetes Prevention Program (DPP) reduced the risk of developing type 2 diabetes by almost 60 percent.4
The program worked, but the challenge for this and other evidence-based interventions targeting chronic diseases is how to reach the people who need it beyond small-scale demonstrations and pilots. As Wayne Giles, director of the Division of Population Health at the CDC’s National Center for Chronic Disease Prevention and Health Promotion, says, “A key challenge in bringing evidence-based interventions to scale is lack of an effective distribution network, especially with chronic diseases, which require more diverse efforts than the typical network of state health agencies.” Just as Dr. Jonas Salk needed the March of Dimes to deliver his polio vaccine to all parts of the United States, researchers today need to find ways to scale up longer-term behavioral interventions.
Enter national nonprofit networks. The YMCA (the Y), the Boys & Girls Clubs of America, OASIS, and other such networks offer a powerful but underused distribution network for scaling up public health interventions. These networks don’t employ doctors and nurses, provide clinical services, or treat patients. What they do offer are features that are both hard to replicate and uniquely suited to the task of changing thinking and behavior on a national scale: a high-profile presence in communities across the nation; large numbers of people already coming through their doors; and staff and volunteers with deep knowledge and expertise about the communities they serve.
To better understand the potential these networks offer to battle chronic disease, in the fall of 2011 we interviewed 50 experts, including public health researchers, practitioners, and leaders of 13 nonprofit networks. In this article we look primarily at the efforts of two networks, the Y and OASIS, to address the pressing national problems of diabetes and childhood obesity, respectively, and we examine how other networks can apply lessons learned from their experiences. We also discuss the steps that leaders of national networks, insurers, the public health research community, and philanthropy can take to scale up proven interventions that will improve the lives and health of tens of millions of Americans.
National Nonprofit Networks
Here’s how the 160-year-old Y is flexing its distribution muscle to address diabetes. Remember the DPP and the extraordinary effort and investment that went into proving its efficacy? By 2006, four years after NIH had unveiled results of its study in The New England Journal of Medicine, few people were receiving the intervention and an estimated 5 to 6 million more had developed the disease. This is when the Y got involved and started offering a carefully crafted adaptation of the DPP at the YMCA of Greater Indianapolis. As of mid-2012, more than 70 local Y associations were delivering the YMCA’s Diabetes Prevention Program, as the Y’s adaptation is known, and more than 6,000 people with prediabetes had been reached. And with approximately 900 local Ys with more than 2,700 facilities around the country serving millions of people of all ages each year, there is plenty of room for further growth.
OASIS, a 30-year-old network that serves adults age 50 and older, is putting its network in the service of efforts to combat childhood obesity. Coordinated Approach to Child Health (CATCH) is an evidence-based curriculum that improves nutrition and increases physical activity among children from preschool through eighth grade. The NIH developed the original curriculum and the University of California, San Diego and the University of Texas later adapted it for delivery by teachers in schools. The data were compelling: After three years of CATCH implementation in Texas schools, 11 percent fewer girls and 9 percent fewer boys receiving the intervention were overweight or obese—exciting news for a health issue that now affects one-third of children nationwide. Although CATCH has gained traction in some schools across the country, it faces the same barrier to adoption as other initiatives competing for precious in-school time.
OASIS offers CATCH a compelling pathway to scale up by using its own volunteers rather than schoolteachers and by using an adaptation of the curriculum designed for after-school time rather than using in-school time. Today, CATCH Healthy Habits, as the OASIS adaptation is known, is being offered by approximately 500 older volunteers at 95 locations across 14 states, reaching more than 3,900 children in grades K through 5. With a network spanning 40 cities across 24 states, there is, as with the Y, plenty of room for further growth.
BRAC, one of the largest NGOs in the world and the second largest employer in Bangladesh after the government, is using its network to reach hundreds of thousands of people afflicted with TB every year. Although TB is a communicable disease, not a chronic one, BRAC’s experience nevertheless provides lessons for nonprofit networks tackling chronic diseases in the United States.
BRAC was established in 1972 as a relief and rehabilitation organization to help resettle refugees following the country’s liberation war. It has since grown to take on a wide variety of other economic development programs. “BRAC was a classic development organization looking at women’s empowerment,” explains Dr. Joseph Rhatigan, director of the Hiatt Global Health Equity Residency Program at Brigham and Women’s Hospital and an assistant professor at Harvard Medical School and the Harvard School of Public Health. “Then it found out that women were defaulting on their microloans for health reasons—tuberculosis—so they decided that they needed to get into the business of fighting TB.” The organization became one of the first to treat TB patients with lay volunteers. Using its 91,000-strong network of community health promoters, known as Shastho Shebikas, BRAC scaled up its treatment model and now treats 100,000 TB patients a year with a success rate of 92 percent.
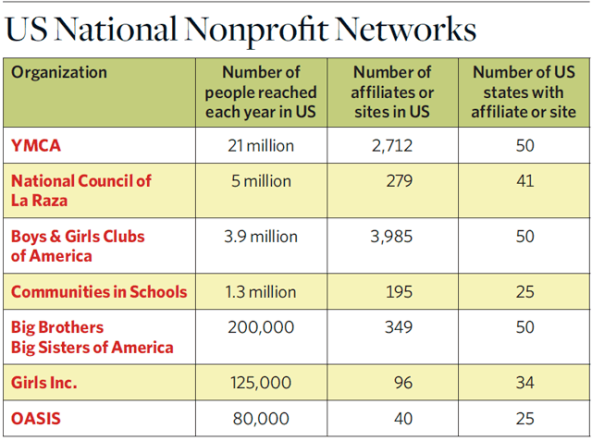
Many nonprofits attempt to scale up their programs. What sets the scaling efforts of the Y, OASIS, and even BRAC apart is that they are using a preexisting distribution infrastructure for something other than its original purpose. And the Y and OASIS are not the only American nonprofits having large distribution networks that can be mobilized. Boys & Girls Clubs of America has 50,000 trained staff and reaches almost 4 million young people annually through its 4,000 clubs; organizations like Girls Inc. and Big Brothers Big Sisters of America (BBBSA) engage many hundreds of thousands of children and youths each year. (See “US National Nonprofit Networks,” below.) Viewed on a national level, nonprofit networks have a reach and impact into day-to-day life in communities that few organizations can rival.
One of the important reasons that national nonprofit networks are particularly valuable in scaling up public health intervention is that they are at once national and local. With deep roots in the community and strong ties to local health care providers, the Y has “an infrastructure that would be hard to replicate,” says Neil Nicoll, president and CEO of YMCA of the USA. The value of those strong local ties is evident at the many sites offering the YMCA’s Diabetes Prevention Program, where the Y partners with local health providers—such as private practice physicians and community health centers—that identify and refer people with prediabetes into the program. In the highly localized business of health care, national nonprofit networks can forge the vital link between clinic and community—a link that is essential to many prevention initiatives.
Scaling Up Interventions
OASIS’s experience with the CATCH Healthy Habits program and the Y’s experience with its adaptation of the DPP suggest that national nonprofit networks must undertake four main tasks to successfully scale up public health interventions. The first is to find an intervention that fits the mission and the capacities of the organization. The next task is to adapt the intervention for community-based delivery. The third is to maintain fidelity to the intervention as it scales up. And the final task is to secure funding to scale up the intervention.
Find an intervention that fits the mission and the capacities of the organization | Before a network can take on the challenge of scaling up public health interventions, its senior leadership must commit the organization to addressing health as a core element of its mission. For the Y, this process unfolded over the course of several years and involved the launching of movement-wide initiatives like Activate America. Other leaders we spoke with indicated that their networks were at an earlier stage in the journey, but that they were actively exploring how they could put their networks in service of the nation’s pressing public health concerns. This was the case with BBBSA, one of the nation’s largest volunteer-supported mentoring networks, operating in all 50 states and in 12 countries around the world, with 240,000 volunteer “Bigs” reaching hundreds of thousands of children each year. “Our history has been centered around mentoring young people. As we move forward, we are open to delivering other types of programs—including health-related programs—that benefit our constituents provided they align well with our vision of all children achieving success in life and are delivered through our mission of mentoring,” says T. Charles Pierson, BBBSA’s president and CEO.
Once a network has committed to improving the health of its members, its first task is to identify an intervention that fits its mission and capacities. Sometimes the match between a network and an intervention is so inspired that it almost seems foreordained. Consider OASIS and CATCH. This match was originally made in 2005 when the Robert Wood Johnson Foundation gave OASIS seed funds to explore intergenerational approaches to health with tested curricula. After surveying the landscape of potential interventions, OASIS staff adapted the University of Texas and University of California, San Diego’s CATCH curriculum, moving delivery of the intervention from an in-school to an after-school setting to allow older adult volunteers to be involved. Evidence from a pilot program demonstrated that eating behaviors and physical activity improved among both students and the older volunteers. OASIS had found an ideal match, an intervention that promoted both healthy living for kids and meaningful engagement for its volunteers.
For the Y, finding the Diabetes Prevention Program was a matter of serendipity. Researchers at the Indiana University School of Medicine were looking to adapt the NIH-tested DPP to a lower-cost, scalable, community-based intervention. The idea of partnering with the Y arose during a chance encounter between the researchers and the vice president of the Y of Greater Indianapolis. For the Y, the program seemed like a natural match: The program fit into the organization’s mission of improving health and well-being, and the evidence showed that the DPP could reduce the incidence of diabetes over the short term. What’s more, the Y had the facilities and corps of potential lifestyle coaches that made it an ideal provider of an intervention centered on behavior change.
The Y recognized an ideal opportunity when it cropped up, but other national networks should not rely on chance encounters. Nonprofit networks can take a systematic approach to identifying suitable health interventions. Surveys of affiliates, members, or both can help identify the health issues most relevant to a network’s constituencies.
Adapt the intervention for community-based delivery | Most preventive and treatment interventions are designed for delivery in clinical settings. Networks, however, will usually need to translate those interventions for delivery in community-based settings. When adapting them, it’s essential that network staff work closely with researchers so that the important features of the intervention are maintained. It is also critical that outcomes are measured to ensure that the network can produce results comparable to those reached in the clinic.
The Y, for example, worked closely with Indiana University researchers for two years to translate the NIH-tested DPP into the YMCA’s Diabetes Prevention Program. The Y program differs in two respects from the original model: It can be delivered to groups rather than one-on-one, and it is offered by trained Y staff rather than by health care professionals. The Y’s investment in adapting the intervention to a community-based setting has paid off: Hundreds of Y lifestyle coaches are delivering the curriculum in classrooms to groups of between eight and 15 adults and achieving results consistent with the original program at approximately 25 percent of the original cost.5
At OASIS, the adaptation of the CATCH curriculum proceeded in two phases—pilot and implementation—with the active support of researchers from the University of Texas. In the first phase not much was changed. OASIS essentially just changed the word “teacher” to “volunteer instructor” in the manual. “It was a very scripted curriculum, and that was helpful since we were using volunteers instead of teachers,” says Peter Holtgrave, national health manager at OASIS. As the program moved into the implementation phase, it became clear that some changes were needed. Some of the games in the original curriculum, for example, were challenging for the older adult volunteers (with an average age in the 70s) and needed to be redesigned. The model has now been codified with one adult volunteer for every five children, and the program can still be implemented without teachers.
Maintain fidelity to the intervention as it scales up | With a proven intervention adapted for delivery in a community-based setting, a network is ready to scale up the program. The Y created a small team devoted exclusively to supporting implementation of the YMCA’s Diabetes Prevention Program at Ys across the network. This team spent one year learning from early implementation efforts and developing resources to support future replications, such as training and marketing materials, and systems to monitor quality and fidelity on an ongoing basis.
The process has not been problem-free. One challenge is that the YMCA of the USA, like many national networks, was accustomed to giving its affiliates a great deal of autonomy to put a localized spin on national initiatives. “Historically, local Ys picked up national programs and adapted them to their local community,” explains Nicoll. “But the reality is that when you’re working with these kinds of evidence-based interventions, you want consistency.” The national office must engage in a delicate dance with local affiliates, respectful of the tensions that inevitably arise when it seeks a degree of standardization that runs counter to the cultural norms that prevail within the networks. Ultimately, however, standardization must win out to maintain fidelity with the intervention.
Girls Inc., a nonprofit network serving more than 125,000 girls in 350 cities, learned a tough and valuable lesson in fidelity and quality assurance when it tackled a long-standing health issue, albeit not a chronic disease. In 1985, Girls Inc. launched the Preventing Adolescent Pregnancy initiative. In 1999, it began a comprehensive evaluation of the program and soon discovered a formidable barrier to impact: The curriculum is meant to be used by affiliates at their own facilities, but many affiliates were delivering the program in schools. That approach made intuitive sense—schools are a great place to reach lots of at-risk girls. But in the school environment, with its many time constraints, the curriculum was being altered and cut into segments that undermined the initiative’s effectiveness. “The girls weren’t getting the real intervention,” says Girls Inc. COO Marcia Brumit Kropf. “And we weren’t getting strong results.”
That finding spurred Girls Inc. to reorient its original intervention to better match the needs of its affiliates. “We learned from the results and now are working to break the curriculum into smaller pieces that can be applied more easily in the real-world context of the schools,” says Kropf. “So in the end we will have an even stronger program that can be implemented with fidelity.” Indeed, the Girls Inc. experience highlights the importance of ongoing evaluation to ensure that outcomes are still being achieved and to allow for course corrections when needed.
Secure funding to scale up the intervention | “Funding is the biggest issue preventing interventions from reaching scale,” according to Jim Krieger, chief of chronic disease and injury prevention at the Seattle & King County Public Health department and professor of public health at the University of Washington. “Most of these evidence-based programs are developed as pilots and are shown to work, and then the funding goes away.”
Government and private foundation funding have important roles to play in the initial stages of creating these programs. OASIS, for example, received early support for the CATCH program from the Robert Wood Johnson Foundation and additional funding to scale up the program from the WellPoint Foundation. But even the largest foundations lack the resources for ongoing investments. For national networks looking to scale up public health interventions, third-party insurance reimbursement may be the answer. Total giving by private foundations has averaged approximately $45 billion annually over the past few years, while total spending on health care stands at around $2.5 trillion annually, or 50 times as much. The source of most of that spending is a vast third-party insurance system that includes many private insurance companies, two big government payment streams (Medicare and Medicaid), and some large self-insured employers like Wal-Mart Stores.
Here, the Y’s experience is particularly instructive. Having benefited from NIH funding for the initial adaptation of the diabetes intervention in Indianapolis, and CDC funding to replicate the program in Louisville, Ky., and 30 other sites, the Y knew it needed to turn to a different source for the next phase of the scaling effort. It achieved a breakthrough when it joined forces with UnitedHealth Group (UHG) in 2009. Impressed by the Y’s ability to achieve the same weight reduction as the original intervention but at a quarter of the cost spent in clinical settings,6 UHG agreed to create a system to reimburse the Y on a pay-for-performance basis for its eligible insured customers who participated in the Y’s program. UHG has since invested millions of dollars in its partnership with the Y, and the Y now partners with a third-party administrator to use a data monitoring and claims generation system that allows it to collect reimbursement from any third-party payer.
Expanding the Model
OASIS’s CATCH Healthy Habits and the YMCA’s Diabetes Prevention Program are more than one-off, fortuitous matches of proven public health interventions and national nonprofit networks. These programs represent a new model for other national nonprofit networks, insurers, public health researchers, and philanthropists who want to scale up evidence-based public health interventions for chronic disease.
Nonprofit networks | Building on the experience gained from the YMCA’s Diabetes Prevention Program, the Y is taking a close look at other evidence-based health interventions that it could potentially scale up such as arthritis self-management programs. It’s rethinking the role of the national organization in providing more leadership on broad health issues, with the aim of capturing and replicating more innovations emerging from local Ys and helping local Ys deliver national programs with greater fidelity than in the past. National leadership recognizes that health interventions are a departure from the services local Ys have traditionally offered—after all, no national network was actually designed to address chronic disease—but it also recognizes that capacity originally developed for other purposes may be exceptionally well suited to this vitally important work.
Other network leaders we spoke with were keen to learn from the experiences of OASIS and the Y. Some, like BBBSA, were at an earlier stage in their own process, still exploring how to expand their missions to include an explicit focus on health. Others were excited about the precedent that the UHG had established in setting up a reimbursement arrangement with the Y, as they could then envision a potentially sustainable funding stream were they to offer chronic disease interventions themselves. At the same time, this type of scaling might not be suitable for all networks. Those best suited are ones with clear distribution platforms—either the physical space within which to deliver a program (like the Y) or a volunteer network that can deliver it in other venues (like OASIS).
Insurers | UHG funded the YMCA’s Diabetes Prevention Program because it was a cost-effective way to treat its customers. Not all chronic disease prevention programs provide such clear-cut financial benefits to insurers. Some private insurers refuse to fund these types of programs because the cost-saving benefits are realized only years later, while the costs to pay for these interventions are incurred in the near term. Because so many people switch insurance coverage, the insurer doesn’t realize the full benefits of the program. The Patient Protection and Affordable Care Act attempts to address this issue by requiring group health plans to cover recommended preventive services. The challenge now is to get interventions like the Y program added to the list of recommended preventive services.
Medicaid and Medicare should follow UHG’s lead. Researchers Ken Thorpe and Zhou Yang have estimated that Medicare could eventually save up to $15 billion if it paid for high-risk people aged 60-64 to enroll in the YMCA’s Diabetes Prevention Program.7 But first, Medicare would have to accept community-based organizations as reimbursable entities akin to traditional health care institutions and overcome its current institutional preference for delivery of chronic disease interventions in clinical settings. Medicare’s recent decision to approve coverage for obesity counseling, but only when it is delivered by a health care professional, suggests that overcoming this bias will be an uphill battle. Nevertheless, there are encouraging signs: In a recent award, the Center for Medicare & Medicaid Innovation provided $11.8 million in funding to the Y in order to demonstrate as much as $53 million in cost savings to the Medicare program over six years through the delivery of the YMCA’s Diabetes Prevention Program. If results are good, a path for public coverage of this program might be more likely.
Public health researchers | Just as successful designers of consumer products and services think about who their customers are and how best to reach them, researchers designing and testing chronic disease interventions should proactively consider how their interventions will reach those most in need. Researchers taking this approach could design interventions for delivery in community-based settings and even tailor them to a national network’s particular capacities.
Funders of public health research, such as the NIH and CDC, can encourage this shift. They can require that researchers outline a compelling path for implementation and dissemination in their funding requests. “If researchers are challenged to think through dissemination at the time the trial is designed, they’re going to head in more practical directions and consider existing distribution platforms in the design of their interventions,” says CDC associate director Janet Collins. “But if they’re never required to do so by research funding sources, then they’re going to come in with a beautiful project that can never be delivered and no one can implement.”
Philanthropists | Although public and private health insurers are often the source of long-term funding, philanthropists can play an important role in getting these programs off the ground. The startup costs can include the research required to adapt or translate a proven intervention for delivery in community-based settings, creating a national training and technical assistance team to support local affiliates that are implementing the solution, and providing money to fund the operations of a few affiliates until funding from insurers can be secured. Philanthropists can also play an important catalyzing role by convening stakeholders to discuss the approach, and cataloging and sharing lessons from those involved in these programs.
Clearly, much remains to be done to prevent and manage major chronic diseases. But there is evidence that national nonprofit networks can make a significant contribution to the effort. If government, philanthropists, public health researchers, and private sector funders support the move, the payoff could be enormous. The lessons learned from participating in one intervention can be applied to the next initiative, until scaling interventions becomes an integral part of the skill set of national networks. As Jonathan Lever, Y-USA’s vice president for health strategy and innovation and architect of Y-USA’s efforts to prevent diabetes, aptly says, “We’re building our distribution muscle, and that muscle will get stronger the more we use it.” The consequences for the nation’s health could be far-reaching and long lasting. With the committed participation of national networks, the battle against 21st-century chronic diseases could one day rival the success of the previous century’s campaigns against infectious diseases.
Read more stories by Taz Hussein & Michaela Kerrissey.


